Pneumonia is the hallmark of severe COVID-19.1 Strain in healthcare systems across the world has forced countless hospitals to conduct grueling triages to decide who gets to be admitted when healthcare saturation was rampant.2 As these decisions are inherently complex, numerous risk scores and predictor factors have been described to aid the attending medical team.3–5 These often include clinical and laboratory values.
One commonly utilized criteria to determine patient severity is the severity of hypoxemia.6 This can be assessed with arterial oxygen pressure (PaO2), PaO2 to inspired fraction of oxygen (FiO2) ratio, arterial oxygen saturation (SatO2), pulse oximeter oxygen saturation (SpO2), SatO2 to FiO2 ratio, SpO2 to FiO2 ratio, and the prescribed oxygen device.7
The use of these criteria for hypoxemia severity in non-intubated patients has been criticized given the expected high inter-patient variability in FiO2, shunt fraction, and physician's choice of oxygenation device and oxygen flow.7 Therefore, relying on these criteria is suboptimal given the low comparability between different patients.
In this study, we aimed to compare the severity of hypoxemia in patients with severe COVID-19 according to oxygenation index arriving at an emergency department.
We performed a retrospective cohort study collecting information on every patient who arrived at the emergency department (ED) of a reference COVID-19 tertiary center between April 1st, 2020, and April 30th, 2021. At arrival, every patient had to go through a triage station where vital signs (including SpO2) were documented before entering the emergency department. Once in the emergency department, all patients who had low SpO2 (usually<92%) received supplemental oxygen. Only nasal cannula and non-rebreathing masks were available at our center. Arterial blood gas analysis was performed in all patients with suspected COVID-19. Generally, FiO2 was estimated heuristically by the treating physician by adding to the baseline FiO2 (21%) 3% for every extra liter of oxygen per minute.8 For example, a patient receiving 2l of minute of supplemental oxygen would have a calculated FiO2 of 27% (21+3*2). SpO2 was obtained at ambient air, while arterial blood gas was obtained almost universally when patients received supplemental oxygen. Given the closeness between SpO2 and blood gas analysis, we believe it is reasonable to assume that the clinical status of the patient is comparable between these two circumstances.
We obtained data about PaO2, SatO2, SpO2, and FiO2, with which we calculated PaO2/FiO2, SatO2/FiO2, and SpO2/FiO2. All SpO2 were taken at triage with a Nihon MU-631RK portable monitor, and as such, were ambient-air (FiO2 21%). SpO2/FiO2 was included to better compare oxygenation indexes. Blood gas analysis was performed in the emergency department with the RADIOMETER ABL90 flex analyzer, which directly measured SatO2 and PaO2. Oxygen device used at the time of the arterial blood gas analysis could not be confidently determined, so it was not included. Since the low reliability of FiO2 is the most criticized aspect of using the oxygenation device as a marker of hypoxia severity, it does not affect our analysis.
We categorized a patient's hypoxemia severity by quintiles of SpO2/FiO2, PaO2/FiO2, and SatO2/FiO2 (from now on referred to as “oxygenation indexes”). Lower values indicate a higher hypoxemia severity. We determined strength of concordance between oxygenation index quintiles with chord diagrams across all three oxygenation index pairs. We calculated Spearman correlation coefficients for the three possible pairs of oxygenation indexes. We built scatterplots and used locally weighted scatterplot smoothing regression to graphically represent the data.
All analyses were conducted with R software version 4.0.0. The study was approved by the Research in Humans ethics committee of the authors’ institution.
A total of 23,049 triage visits occurred during the study period, corresponding to 19,644 individual patients. Of these, 8123 were due to suspected COVID-19. Among 4663 patients that were finally admitted to the ED, arterial blood gas analysis was obtained for 2960 patients.
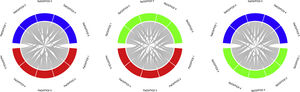
Median FiO2 was 0.34 (inter-quartile range [IQR] 0.25–0.60), PaO2 68mmHg (57–84), SatO2 94% (91–97), SpO2 83% (73–88), PaO2/FiO2 211 (124–281), SatO2/FiO2 274 (160–364), and SpO2/FiO2 395 (348–419). Correlation among oxygenation indexes is shown in Fig. 1. A strong correlation was seen between PaO2/FiO2 & SpO2/FiO2 (rho=0.6, p<0.001), and SatO2/FiO2 & SpO2/FiO2 (rho=0.65, p<0.001), while a very strong correlation was seen between PaO2/FiO2 & SatO2/FiO2 (rho=0.88, p<0.001). None of the variable pairs showed a linear relationship. All oxygenation indexes showed a considerable cross-over among quintiles (Fig. 2), with only 785 (26.5%) patients being in the same severity quintile across all indexes.
Variability of concordance between oxygenation indexes’ quintiles. SpO2: oxygen saturation with pulse oximeter; PaO2: oxygen pressure in arterial blood; SatO2: oxygen saturation in arterial blood; FiO2: fraction of inspired oxygen. (A) Shows relation between PaO2/FiO2 and SatO2/FiO2, (B) shows relation between PaO2/FiO2 and SpO2/FiO2, and (C) shows relation between SpO2/FiO2 and SatO2/FiO2. Numbers represent the respective quintile (“PaO2/FiO2 1” represents the first quintile of said variable).
Our study shows there is considerable heterogeneity when classifying hypoxemia severity with different oxygenation indexes. While good correlation was observed among the three evaluated pairs, the lower correlation between SpO2/FiO2 and the others could be due to inaccuracy of pulse oximeters when used in patients with low oxygen saturation, physician imprecision when estimating FiO2, and/or mixed blood in the gas analysis.9 It is likely multiple factors are involved in most cases, which is consistent with the previously mentioned concerns.7 For example, if solely based on SpO2 at triage, a patient could be wrongly classified as having a more severe disease, giving preference to a patient in better condition. Also, follow up could be hard if it is done only with oxygenation parameters. The morning medical team could classify the patient with a given severity with blood gas analysis, while the evening group could use a pulse oximeter and determine intubation is indicated.
Degree of hypoxemia is not a good measure when considered by itself in non-intubated patients with COVID-19 pneumonia, as considerable variation occurs depending on whether pulse oximetry or blood gas analysis is utilized.
Data availabilityCode used for the analysis is freely available at https://github.com/isaac-nunez/Oxygenation_indexes. Data will be made available upon reasonable request to the corresponding author.
Sources of fundingThis research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Conflicts of interestThe authors have no conflicts of interest.
The authors would like to thank the triage personnel of their institution for their invaluable work during the pandemic, as well as an anonymous reviewer for helpful comments to improve the manuscript.