Infections have become one of the main complications of patients with severe SARS-CoV-2 pneumonia admitted in ICU. Poor immune status, frequent development of organic failure requiring invasive supportive treatments, and prolonged ICU length of stay in saturated structural areas of patients are risk factors for infection development. The Working Group on Infectious Diseases and Sepsis GTEIS of the Spanish Society of Intensive Medicine and Coronary Units SEMICYUC emphasizes the importance of infection prevention measures related to health care, the detection and early treatment of major infections in the patient with SARS-CoV-2 infections. Bacterial co-infection, respiratory infections related to mechanical ventilation, catheter-related bacteremia, device-associated urinary tract infection and opportunistic infections are review in the document.
Las infecciones se han convertido en una de las principales complicaciones de los pacientes con neumonía grave por SARS-CoV-2 que ingresan en UCI. El deficiente estado inmunitario, el desarrollo frecuente de fracaso orgánico con necesidad de tratamientos de soporte invasivos y las estancias prolongadas en áreas estructurales en gran medida saturadas de enfermos son factores de riesgo para el desarrollo de infecciones. El Grupo de Trabajo de Enfermedades Infecciosas y Sepsis GTEIS de la Sociedad Española de Medicina Intensiva y Unidades Coronarias SEMICYUC enfatiza la importancia de las medidas de prevención de infecciones relacionadas con los cuidados sanitarios, y de la detección y tratamiento precoz de las principales infecciones en el paciente con infección por SARS-CoV-2. La coinfección bacteriana, las infecciones respiratorias relacionadas con la ventilación mecánica, bacteriemia relacionada con el catéter, infección del tracto urinario asociado a dispositivo e infecciones oportunistas son desarrolladas.
Over one year has gone by since the description of the first cases of respiratory infection due to the SARS-CoV-2 coronavirus.1 The Spanish national COVID-19/SEMICYUC registry of cases admitted to Intensive Care Units (ICUs) in Spain has evidenced a high percentage of patients who develop organ failure (100% respiratory, 44% cardiovascular and 30% renal), with long ICU stays (14 days [range 8–26]) and a mortality rate of 32.6% according to the results corresponding to the first 2200 patients published.2 Potere et al., in a systematic review and meta-analysis of the first series of patients in the ICU, documented a mortality rate of 34% that increased to 83% among patients on mechanical ventilation (MV)3 – a figure significantly higher than that observed in the COVID-19/SEMICYUC registry.2
It can be affirmed that the empirical treatments with scant scientific evidence used in the early stages of the pandemic unfortunately yielded no benefits and did not modify the ominous course of the severe cases seen in the ICU.4 Likewise, the first data generated by the ENVIN-COVID registry, based on the analysis of 1525 patients with COVID-19 admitted to intensive care between 15 March and 30 May, showed that 50% of the patients had suffered one or more infections related to medical care, and that the frequencies of the different controlled infections had multiplied between two- and four-fold (ENVIN-COVID report, 2020).5 It therefore seems prudent to place emphasis on measures for the prevention of infections in the ICU, and on their early detection, with the aim of providing adequate and early treatment in the difficult challenge of combating the high associated mortality.
With this aim in mind, the Working Group on Infectious Diseases and Sepsis (Grupo de Trabajo de Enfermedades Infecciosas y Sepsis [GTEIS]) of the Spanish Society of Intensive and Critical Care Medicine and Coronary Units (Sociedad Española de Medicina Intensiva, Crítica y Unidades Coronarias [SEMICYUC]), on occasion of its latest ordinary meeting, agreed to carry out a literature review on the state of the art and offer a series of treatment recommendations established by the authors of this document, which were selected by the coordinators of the Working Group on the basis of their experience in infectious diseases.
Role of immune modulating treatments in nosocomial infectionDuring the first months of the pandemic, the lowering of a dysregulated immune response was considered to be a potential therapeutic strategy. As a result, and even in the absence of clear scientific evidence, frequent use was made of a range of antiinflammatory drugs and immune modulators such as glucocorticoids, inhibitors of interleukins and/or their receptors, antimalarials, antimitotic agents, calcineurin inhibitors, etc. However, these drugs are not without side effects – one of the most serious of which is an enhanced susceptibility to superinfections in the hospital setting.
Knowledge about the effect of corticosteroids upon the development of superinfections in patients with SARS-CoV-2 infection is presently limited. A meta-analysis of the clinical trials that have evaluated corticosteroid use in critical patients with SARS-CoV-2 infection carried out by the World Health Organization (WHO) concluded that the included studies contributed little information on the adverse effects, and that no meta-analysis of the data was possible.6 Nevertheless, some studies suggested that the use of corticosteroids may be associated to an increased risk of certain infections such as bacteremias, particularly when these drugs are combined with other immunosuppressors.7
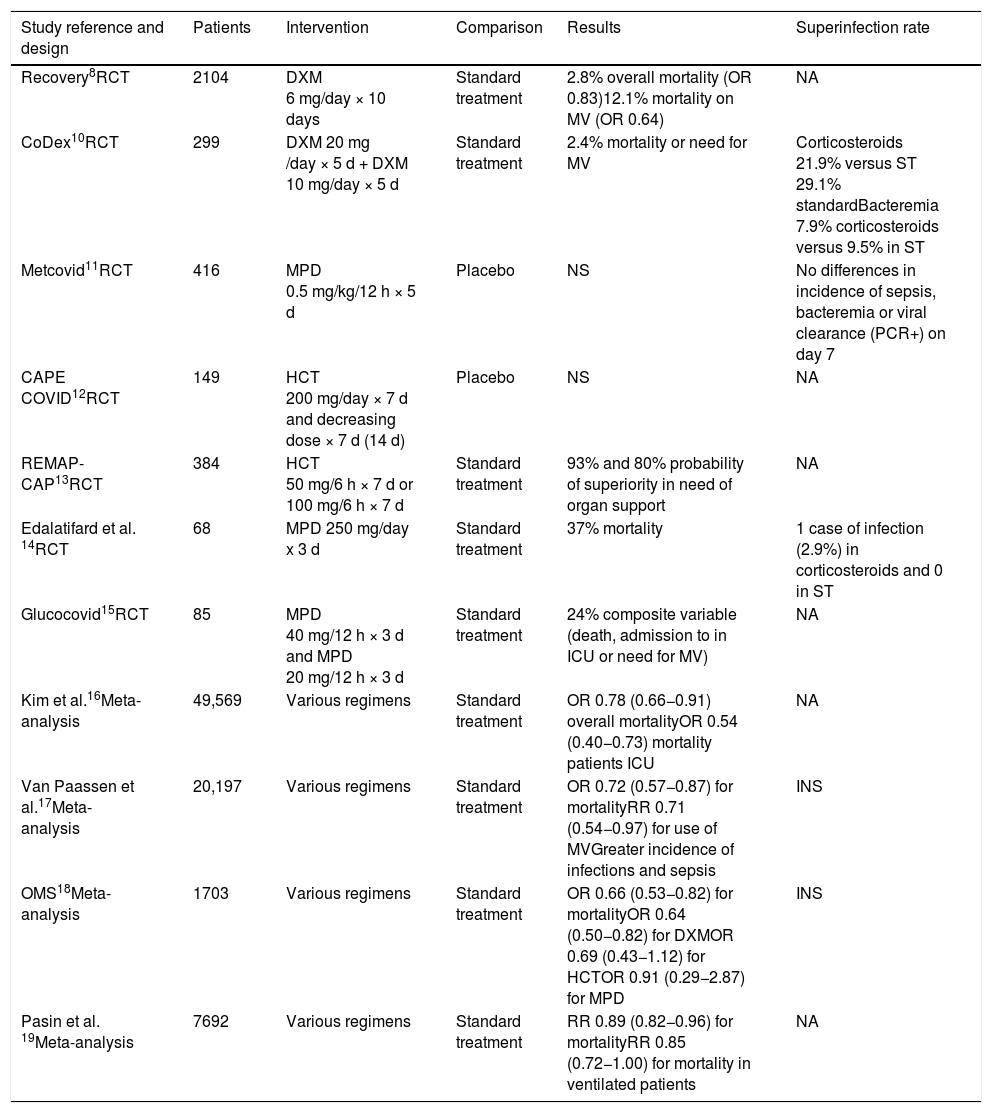
Based on the evidence available at the time of drafting of this document, and following the guidelines of the WHO, among others, the use of corticosteroids – preferably dexamethasone – is recommended for the treatment of patients with severe COVID-19.8 It should be considered that although patients with milder respiratory failure could benefit from such treatment, the maximum benefits have been observed in critical patients subjected to mechanical ventilation (odds ratio [OR] 0.66 [95%CI: 0.53−0.82]). Monedero et al.9 reported that the early administration of corticosteroids, within the first 48 h of admission to the ICU is associated to a lesser risk of nosocomial infection (56.3% of cases; OR 1.39, p = 0.05) than when such treatment is provided on a later basis (69.9% of cases; OR = 2.5 p < 0.001) – though the risk of infection is even lower among those patients who never received the drug (48.2% of the cases, OR = 1). Table 110–19 summarizes the main studies on the use of corticosteroids and their association to the development of infections. As regards the type of drug and dose, dexamethasone is preferentially advised, at a dose of 6–7.5 mg/day between 7 and 10 days, since it is the drug substance used in a larger number of studies and which has been found to afford statistically significant clinical benefits.8
Summary of studies on the effect of corticosteroids in SARS-CoV-2 pneumonia. Design, clinical outcomes and association to the development of infection.
| Study reference and design | Patients | Intervention | Comparison | Results | Superinfection rate |
|---|---|---|---|---|---|
| Recovery8RCT | 2104 | DXM 6 mg/day × 10 days | Standard treatment | 2.8% overall mortality (OR 0.83)12.1% mortality on MV (OR 0.64) | NA |
| CoDex10RCT | 299 | DXM 20 mg /day × 5 d + DXM 10 mg/day × 5 d | Standard treatment | 2.4% mortality or need for MV | Corticosteroids 21.9% versus ST 29.1% standardBacteremia 7.9% corticosteroids versus 9.5% in ST |
| Metcovid11RCT | 416 | MPD 0.5 mg/kg/12 h × 5 d | Placebo | NS | No differences in incidence of sepsis, bacteremia or viral clearance (PCR+) on day 7 |
| CAPE COVID12RCT | 149 | HCT 200 mg/day × 7 d and decreasing dose × 7 d (14 d) | Placebo | NS | NA |
| REMAP-CAP13RCT | 384 | HCT 50 mg/6 h × 7 d or 100 mg/6 h × 7 d | Standard treatment | 93% and 80% probability of superiority in need of organ support | NA |
| Edalatifard et al. 14RCT | 68 | MPD 250 mg/day x 3 d | Standard treatment | 37% mortality | 1 case of infection (2.9%) in corticosteroids and 0 in ST |
| Glucocovid15RCT | 85 | MPD 40 mg/12 h × 3 d and MPD 20 mg/12 h × 3 d | Standard treatment | 24% composite variable (death, admission to in ICU or need for MV) | NA |
| Kim et al.16Meta-analysis | 49,569 | Various regimens | Standard treatment | OR 0.78 (0.66−0.91) overall mortalityOR 0.54 (0.40−0.73) mortality patients ICU | NA |
| Van Paassen et al.17Meta-analysis | 20,197 | Various regimens | Standard treatment | OR 0.72 (0.57−0.87) for mortalityRR 0.71 (0.54−0.97) for use of MVGreater incidence of infections and sepsis | INS |
| OMS18Meta-analysis | 1703 | Various regimens | Standard treatment | OR 0.66 (0.53−0.82) for mortalityOR 0.64 (0.50−0.82) for DXMOR 0.69 (0.43−1.12) for HCTOR 0.91 (0.29−2.87) for MPD | INS |
| Pasin et al. 19Meta-analysis | 7692 | Various regimens | Standard treatment | RR 0.89 (0.82−0.96) for mortalityRR 0.85 (0.72−1.00) for mortality in ventilated patients | NA |
d: days; DXM: dexamethasone; RCT: randomized clinical trial; HCT: hydrocortisone; INS: insufficient information; MPD: methylprednisolone; NA: no data available; NS: nonsignificant; OR: odds ratio; P: placebo; RR: relative risk; MV: mechanical ventilation.
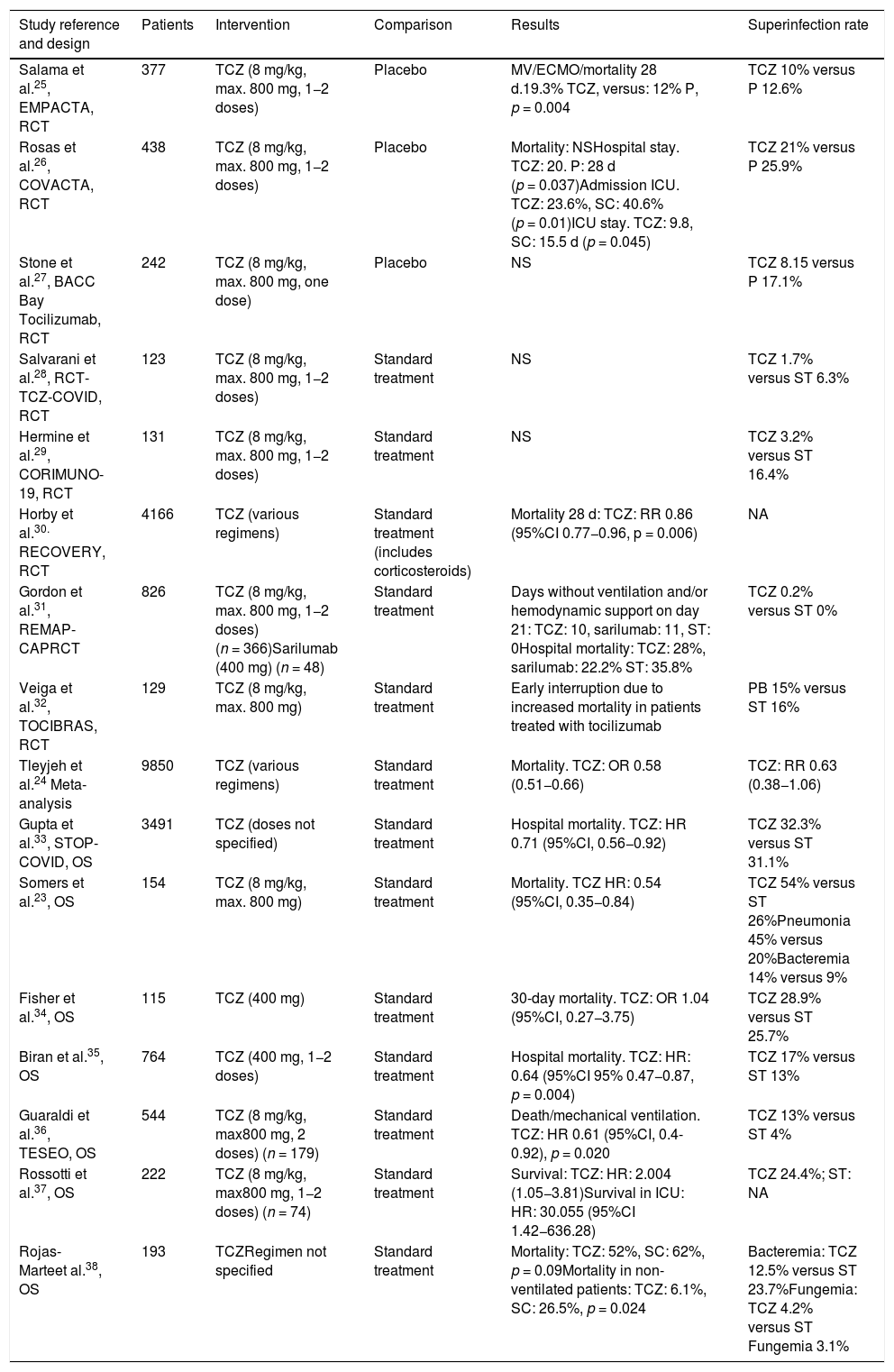
The use of tocilizumab could be justified to reduce the inflammatory component associated with COVID-19, though as a deleterious effect, the drug could interfere with the host immune response to viral replication. Its prescription in this disease condition is therefore controversial, with evidence both in favor and against its use. The main side effect of tocilizumab is a predisposition to develop infections. Data obtained from post-authorization experience with the drug indicate that the most frequent complication is upper airway infections, including pneumonia (>10% of the patients), followed by cellulitis and herpetic reactivations (1–10%) and, more rarely, diverticulitis (<1%).20,21 Between 3–7% of all patients may develop a potentially serious infection.22 In the context of COVID-19, a recent study published by Somers et al.23 evidenced that the administration of tocilizumab in a cohort of 154 patients subjected to mechanical ventilation was associated to a greater proportion of superinfections (54% versus 26%; p < 0.001). Pneumonia (45%) and bacteremia (14%) were the most frequent conditions, and the most commonly isolated organism was Staphylococcus aureus (S. aureus) (51% of the cases) – though no differences were observed in the 28-day mortality rate between those patients treated with tocilizumab with or without superinfection [22% versus 15%; p = 0.42]. However, most of the studies have recorded no higher incidence of infection in those patients who received the drug. In the largest meta-analysis to date, Tleyjeh et al., comprising a total 9850 patients,24 found the use of tocilizumab to imply no higher nosocomial infection rate than that recorded in the control group, though the drug was associated to a lesser mortality rate and/or need for mechanical ventilation. In the largest clinical trial to date – the RECOVERY study – a decrease in mortality was observed (relative risk [RR] 0.86 [95%CI: 0.77−0.96]; p = 0.006) in the subgroup of patients that received tocilizumab, with C-reactive protein >75 and pulsioximetry <92%. Of note is the fact that 82% of the patients received corticosteroids in both arms of the study, and no data were moreover provided on the incidence of nosocomial infection. Table 2 summarizes the main studies on tocilizumab and its association to the appearance of infections.25–38
Summary of studies on the effect of tocilizumab in SARS-CoV-2 pneumonia. Design, clinical outcomes and association to the development of infection.
| Study reference and design | Patients | Intervention | Comparison | Results | Superinfection rate |
|---|---|---|---|---|---|
| Salama et al.25, EMPACTA, RCT | 377 | TCZ (8 mg/kg, max. 800 mg, 1−2 doses) | Placebo | MV/ECMO/mortality 28 d.19.3% TCZ, versus: 12% P, p = 0.004 | TCZ 10% versus P 12.6% |
| Rosas et al.26, COVACTA, RCT | 438 | TCZ (8 mg/kg, max. 800 mg, 1−2 doses) | Placebo | Mortality: NSHospital stay. TCZ: 20. P: 28 d (p = 0.037)Admission ICU. TCZ: 23.6%, SC: 40.6% (p = 0.01)ICU stay. TCZ: 9.8, SC: 15.5 d (p = 0.045) | TCZ 21% versus P 25.9% |
| Stone et al.27, BACC Bay Tocilizumab, RCT | 242 | TCZ (8 mg/kg, max. 800 mg, one dose) | Placebo | NS | TCZ 8.15 versus P 17.1% |
| Salvarani et al.28, RCT-TCZ-COVID, RCT | 123 | TCZ (8 mg/kg, max. 800 mg, 1−2 doses) | Standard treatment | NS | TCZ 1.7% versus ST 6.3% |
| Hermine et al.29, CORIMUNO-19, RCT | 131 | TCZ (8 mg/kg, max. 800 mg, 1−2 doses) | Standard treatment | NS | TCZ 3.2% versus ST 16.4% |
| Horby et al.30. RECOVERY, RCT | 4166 | TCZ (various regimens) | Standard treatment (includes corticosteroids) | Mortality 28 d: TCZ: RR 0.86 (95%CI 0.77−0.96, p = 0.006) | NA |
| Gordon et al.31, REMAP-CAPRCT | 826 | TCZ (8 mg/kg, max. 800 mg, 1−2 doses)(n = 366)Sarilumab (400 mg) (n = 48) | Standard treatment | Days without ventilation and/or hemodynamic support on day 21: TCZ: 10, sarilumab: 11, ST: 0Hospital mortality: TCZ: 28%, sarilumab: 22.2% ST: 35.8% | TCZ 0.2% versus ST 0% |
| Veiga et al.32, TOCIBRAS, RCT | 129 | TCZ (8 mg/kg, max. 800 mg) | Standard treatment | Early interruption due to increased mortality in patients treated with tocilizumab | PB 15% versus ST 16% |
| Tleyjeh et al.24 Meta-analysis | 9850 | TCZ (various regimens) | Standard treatment | Mortality. TCZ: OR 0.58 (0.51−0.66) | TCZ: RR 0.63 (0.38−1.06) |
| Gupta et al.33, STOP-COVID, OS | 3491 | TCZ (doses not specified) | Standard treatment | Hospital mortality. TCZ: HR 0.71 (95%CI, 0.56−0.92) | TCZ 32.3% versus ST 31.1% |
| Somers et al.23, OS | 154 | TCZ (8 mg/kg, max. 800 mg) | Standard treatment | Mortality. TCZ HR: 0.54 (95%CI, 0.35−0.84) | TCZ 54% versus ST 26%Pneumonia 45% versus 20%Bacteremia 14% versus 9% |
| Fisher et al.34, OS | 115 | TCZ (400 mg) | Standard treatment | 30-day mortality. TCZ: OR 1.04 (95%CI, 0.27−3.75) | TCZ 28.9% versus ST 25.7% |
| Biran et al.35, OS | 764 | TCZ (400 mg, 1−2 doses) | Standard treatment | Hospital mortality. TCZ: HR: 0.64 (95%CI 95% 0.47−0.87, p = 0.004) | TCZ 17% versus ST 13% |
| Guaraldi et al.36, TESEO, OS | 544 | TCZ (8 mg/kg, max800 mg, 2 doses) (n = 179) | Standard treatment | Death/mechanical ventilation. TCZ: HR 0.61 (95%CI, 0.4-0.92), p = 0.020 | TCZ 13% versus ST 4% |
| Rossotti et al.37, OS | 222 | TCZ (8 mg/kg, max800 mg, 1−2 doses) (n = 74) | Standard treatment | Survival: TCZ: HR: 2.004 (1.05−3.81)Survival in ICU: HR: 30.055 (95%CI 1.42−636.28) | TCZ 24.4%; ST: NA |
| Rojas-Marteet al.38, OS | 193 | TCZRegimen not specified | Standard treatment | Mortality: TCZ: 52%, SC: 62%, p = 0.09Mortality in non-ventilated patients: TCZ: 6.1%, SC: 26.5%, p = 0.024 | Bacteremia: TCZ 12.5% versus ST 23.7%Fungemia: TCZ 4.2% versus ST Fungemia 3.1% |
d: days; RCT: randomized clinical trial; ECMO: extracorporeal membrane oxygenation; OS: observational study; INS: insufficient information; NA: no data available; NS: nonsignificant; OR: odds ratio; P: placebo; RR: relative risk; TCZ: tocilizumab; MV: mechanical ventilation; NIV: noninvasive ventilation.
Lastly, it must be remembered that tocilizumab inhibits the acute phase reactants produced in the liver, such as C-reactive protein,39 which therefore limits their usefulness in the diagnosis and assessment of treatment response in patients with nosocomial infection and sepsis.
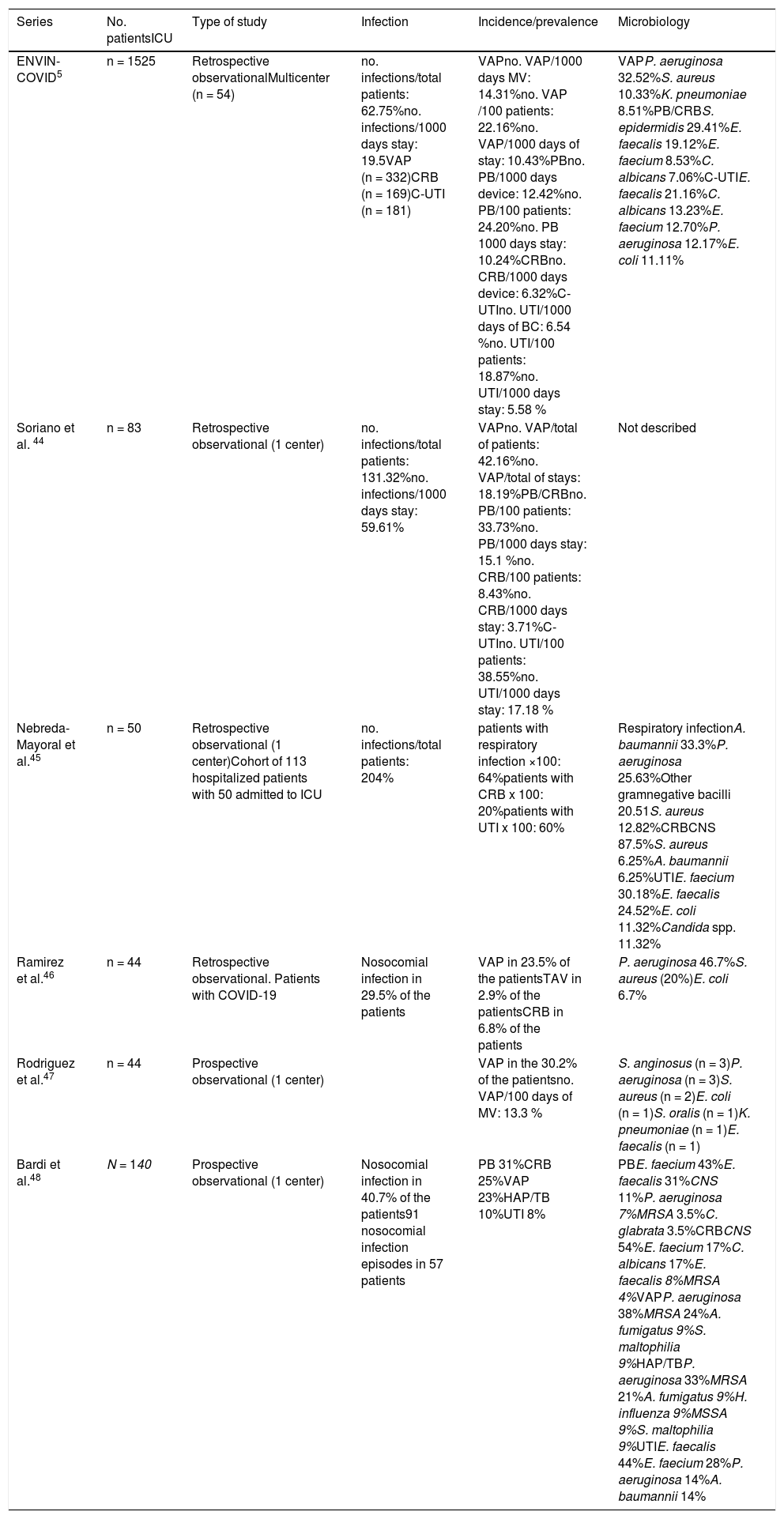
Prevention of infections related to medical careThe adoption of the recommendations of the Zero Projects has proven to be effective in reducing the appearance of infections related to medical care during patient admission to the ICU in Spain.40,41 The statistics on the different infections related to the use of invasive devices published by the ENVIN registry in the year 201942 were more than adequately compliant with the quality standards of the SEMICYUC.43 During the early phases of the COVID-19 pandemic, the application of contingency plans designed to address the growing healthcare demands, implied the introduction of important structural, functional and human changes that posed barriers for complying with the established prevention measures. In recent months (Table 3), important increments have been reported in the incidence of infections related to medical care among the COVID-19 patients admitted to different Spanish ICUs.44–48 The Critical Patients Safety Projects Advisory Council has recently published a document49 proposing adaptation of the recommendations of the Zero Projects during the SARS-CoV-2 pandemic. Appendix B summarizes the measures contemplated in the mentioned document, and which are complemented by adaptation of the management of invasive devices during patient transfer or during placement in prone decubitus, the prevention of pressure ulcers, and the application of body hygiene.
Reported incidence of infectious complications in series of patients with severe SARS-CoV-2 pneumonia.
| Series | No. patientsICU | Type of study | Infection | Incidence/prevalence | Microbiology |
|---|---|---|---|---|---|
| ENVIN-COVID5 | n = 1525 | Retrospective observationalMulticenter (n = 54) | no. infections/total patients: 62.75%no. infections/1000 days stay: 19.5VAP (n = 332)CRB (n = 169)C-UTI (n = 181) | VAPno. VAP/1000 days MV: 14.31%no. VAP /100 patients: 22.16%no. VAP/1000 days of stay: 10.43%PBno. PB/1000 days device: 12.42%no. PB/100 patients: 24.20%no. PB 1000 days stay: 10.24%CRBno. CRB/1000 days device: 6.32%C-UTIno. UTI/1000 days of BC: 6.54 %no. UTI/100 patients: 18.87%no. UTI/1000 days stay: 5.58 % | VAPP. aeruginosa 32.52%S. aureus 10.33%K. pneumoniae 8.51%PB/CRBS. epidermidis 29.41%E. faecalis 19.12%E. faecium 8.53%C. albicans 7.06%C-UTIE. faecalis 21.16%C. albicans 13.23%E. faecium 12.70%P. aeruginosa 12.17%E. coli 11.11% |
| Soriano et al. 44 | n = 83 | Retrospective observational (1 center) | no. infections/total patients: 131.32%no. infections/1000 days stay: 59.61% | VAPno. VAP/total of patients: 42.16%no. VAP/total of stays: 18.19%PB/CRBno. PB/100 patients: 33.73%no. PB/1000 days stay: 15.1 %no. CRB/100 patients: 8.43%no. CRB/1000 days stay: 3.71%C-UTIno. UTI/100 patients: 38.55%no. UTI/1000 days stay: 17.18 % | Not described |
| Nebreda-Mayoral et al.45 | n = 50 | Retrospective observational (1 center)Cohort of 113 hospitalized patients with 50 admitted to ICU | no. infections/total patients: 204% | patients with respiratory infection ×100: 64%patients with CRB x 100: 20%patients with UTI x 100: 60% | Respiratory infectionA. baumannii 33.3%P. aeruginosa 25.63%Other gramnegative bacilli 20.51S. aureus 12.82%CRBCNS 87.5%S. aureus 6.25%A. baumannii 6.25%UTIE. faecium 30.18%E. faecalis 24.52%E. coli 11.32%Candida spp. 11.32% |
| Ramirez et al.46 | n = 44 | Retrospective observational. Patients with COVID-19 | Nosocomial infection in 29.5% of the patients | VAP in 23.5% of the patientsTAV in 2.9% of the patientsCRB in 6.8% of the patients | P. aeruginosa 46.7%S. aureus (20%)E. coli 6.7% |
| Rodriguez et al.47 | n = 44 | Prospective observational (1 center) | VAP in the 30.2% of the patientsno. VAP/100 days of MV: 13.3 % | S. anginosus (n = 3)P. aeruginosa (n = 3)S. aureus (n = 2)E. coli (n = 1)S. oralis (n = 1)K. pneumoniae (n = 1)E. faecalis (n = 1) | |
| Bardi et al.48 | N = 140 | Prospective observational (1 center) | Nosocomial infection in 40.7% of the patients91 nosocomial infection episodes in 57 patients | PB 31%CRB 25%VAP 23%HAP/TB 10%UTI 8% | PBE. faecium 43%E. faecalis 31%CNS 11%P. aeruginosa 7%MRSA 3.5%C. glabrata 3.5%CRBCNS 54%E. faecium 17%C. albicans 17%E. faecalis 8%MRSA 4%VAPP. aeruginosa 38%MRSA 24%A. fumigatus 9%S. maltophilia 9%HAP/TBP. aeruginosa 33%MRSA 21%A. fumigatus 9%H. influenza 9%MSSA 9%S. maltophilia 9%UTIE. faecalis 44%E. faecium 28%P. aeruginosa 14%A. baumannii 14% |
PB: primary bacteremia; CRB: catheter-related bacteremia; C-UTI: bladder catheter-related urinary tract infection; HAP: hospital-acquired pneumonia; VAP: ventilator-associated pneumonia; MSSA: methicillin-sensitive S. aureus; MRSA: methicillin-resistant S. aureus; CNS: coagulase-negative Staphylococcus; BC: bladder catheter; TB: tracheobronchitis.
Despite the recording of a low incidence of bacterial coinfection in hospitalized patients with SARS-CoV-2,50 the incidence recorded in the ICU according to the COVID-19/SEMICYUC registry was 9.3%.2 The recommendation provided in this document seeks to draw attention to the possibility of such infection, in the awareness of the risk and increase in mortality associated with delays in treating complications of this kind.51
A proactive diagnosis of coinfection in clinically severe presentations should be a priority concern. The classical clinical criteria of fever, respiratory failure and radiological infiltration are common to viral pneumonia, and therefore are unable to differentiate the possibility of bacterial coinfection. The distinguishing clinical feature is probably the fact that secretions are typically scarce or inexistent in the early stages of viral pneumonia without coinfection. Patients admitted to the ICU may come directly from the Emergency Department or from the hospital ward. In the latter case, and depending on the number of days spent in the ward, the previous treatments used and the invasive devices employed, we may consider the possibility of infection related to medical care, though in any case the recommendation to actively assess infectious complications upon arrival in the Unit remains the same.
Although procalcitonin values alone are not advised for deciding the start of antibiotic treatment,52 procalcitonin is a more specific tool than C-reactive protein, and in conjunction with the clinical and radiological data may help in considering the possibility of coinfection. Accordingly, it is advisable to determine procalcitonin upon admission to the UCI, and in this regard some authors have proposed a cut-off concentration of <0.1 µg/l as suggestive of viral pneumonia,53,54 in view of its high negative predictive value. In addition, it will be useful to know the subsequent clearance of this marker with a view to deciding the suspension of empirical antibiotic treatment. We thus advise the collection of respiratory samples upon admission to the ICU (at least a tracheal aspirate in intubated patients and a sputum sample in non-intubated patients). Table 4 details the recommended microbiology laboratory tests for studying the respiratory samples.
Microbiological study of respiratory samples.
| Gram staining and microbiological culture |
| Determination of presence of coronavirus |
| PCR testing for virus influenza and RSV |
| KOH and/or calcofluor staining |
| Real-time PCR testing for Aspergillus* |
| LFA*/Galactomannan antigen |
| Staining and culture for mycobacteria |
LFA: lateral flow assay.
Langford et al. evaluated the presence of bacterial coinfection in a meta-analysis55 of over 3000 patients. A total of 3.5% of the patients presented coinfection – a figure lower than that reported in patients with infection due to influenza virus. In relation to the critically ill, the authors analyzed the data of 5 studies documenting coinfection in 14 out of a total of 144 patients (9.7%). No etiological data in critical cases were provided, though it seems reasonable to consider Streptococcus pneumoniae and S. aureus as possibly being the most frequent bacteria in community-acquired pneumonia. Based on these data, it has been debated whether empirical treatment should be started or not. What is clear is that the potential presence of bacterial coinfection should be investigated in all cases. A strategy which in our opinion seems reasonable is to start antibiotic treatment considering the most frequent pathogens in community-acquired pneumonia, and to adjust or suspend treatment after 48–72 h conditioned to the microbiological results obtained. If empirical antibiotic therapy is started, we recommend combination treatment in the form of a third-generation cephalosporin such as ceftriaxone or cefotaxime associated to levofloxacin or azithromycin, though a fifth-generation cephalosporin such as ceftaroline could also be prescribed.
Ventilator-associated respiratory infectionVentilator-associated respiratory infection (VARI), including ventilator-associated tracheobronchitis and ventilator-associated pneumonia (VAP), are common in critical patients subjected to mechanical ventilation56. Patients with pneumonia due to SARS-CoV-2 could be at an increased risk of VARI,57 due to acute respiratory distress syndrome (ARDS) and the long duration of mechanical ventilation. Acute respiratory distress syndrome is a well-known risk factor for VAP,58,59 and its incidence in ventilated patients with SARS-CoV-2 pneumonia is reportedly high (42–89%).60,61 Likewise, SARS-CoV-2 is responsible for alterations of host immune response.
Recently, two Spanish groups62,63 have published their experience, with an incidence of almost 52% referred to infections acquired in the ICU – respiratory foci being the most common presentation in both series, and implying significantly higher mortality in one of the studies.62Pseudomonas aeruginosa was the most frequently isolated microorganism.30,40
Rouze et al.64 carried out a multicenter study to determine the relationship between SARS-CoV-2 infection and the incidence and etiology of VARI. The study was carried out in 36 ICUs in Europe (28 in France, 3 in Spain, 3 in Greece, 1 in Portugal and 1 in Ireland). The interesting feature of this study is that it included the same number of patients on mechanical ventilation per center with SARS-CoV-2 infection, influenza infection or no viral infection. The main finding was that the incidence of ventilator-associated tracheobronchitis and VAP was greater in the patients with SARS-CoV-2 than in the other two groups (influenza infection or no viral infection). Gramnegative bacilli were responsible for most of the first VARI episodes in all three study groups. P. aeruginosa, Enterobacter spp. and Klebsiella spp. were the most commonly identified bacteria. The percentage of patients with VARI involving multiresistant bacteria was lower in pneumonia due to SARS-CoV-2 than in the other two groups.
The choice of empirical and/or guided treatment should be based on the clinical entity and the severity of presentation, the presence of risk factors for infection due to a multiresistant microorganism, the existence of comorbidities, and knowledge of the local flora and multiresistance rates of the center involved, according to the proposed algorithm.65 The increase in bacterial resistances and the high incidence of infections involving gramnegative bacilli such as Klebsiella spp. and Pseudomonas spp., lead us to consider empirical treatments with activity against this etiological profile, including carbapenems (for which the appearance of resistances is increasing), ceftazidime-avibactam and ceftolozane-tazobactam, whose spectrum of action covers these possibilities. The duration of treatment has not been clearly established, and in this type of infection in particular, the decision must be individualized, in view of the important lung damage caused. Likewise, we always must consider the possibility of shortening both the duration of treatment and tapering of the regimen, based on the use of scales such as the Clinical Pulmonary Infection Score (CPIS), and biomarkers such as C-reactive protein and particularly procalcitonin65 in combination may be of help.
Table 5 summarizes the recommendations on the management of VAP in patients with COVID-19.
Recommendations for the management of ventilator-associated respiratory infections in critical patients with SARS-CoV-2 pneumonia.
| - Due to their high incidence, a strong level of suspicion should be maintained, with the early start of antibiotic treatments |
| - Empirical and/or guided treatment should be based on the clinical entity and the severity of presentation, the presence of risk factors for infection due to a multiresistant microorganism, the existence of comorbidities, the possible use of rapid techniques, and knowledge of the local flora and multiresistance rates of the center |
| - Initial empirical combination coverage should be provided with antipseudomonal betalactams, including ceftazidime – avibactam or ceftolozane – tazobactam plus quinolones or aminoglycosides |
| - Empirical coverage of MRSA is not necessary if its incidence in the center is low or inexistent |
| - In order to avoid unwarranted antibiotic use, treatment should be suspended if infection is not documented |
| - In guided treatment, monotherapy is advised, with the possibility of reducing the spectrum of action |
| - The duration of treatment should be individualized, and longer therapy may be necessary in these patients, depending on the clinical course, biomarkers use and the presence of multiresistances |
The Bacteremia Zero Project has reduced the incidence of catheter-related bacteremia (CRB),40 though in the moments of maximum critical care bed occupation and expansion it has been difficult to maintain compliance with the measures recommended by this and by other similar projects in our Units.49 A greater incidence of nosocomial bacteremia has been observed in COVID-19 patients admitted to hospital than in non-COVID-19 patients (5.3% versus 1.4%; p < 0.001), and admission to the ICU has moreover been identified as a risk factor.66 The ENVIN-COVID report of 2020 has described an incidence of 6.32 cases per 1000 days of central venous catheter,5 which is much higher than usual in our Units. Similar and even poorer results have been obtained in other studies. Giacobbe et al. documented an incidence of nosocomial bacteremia of 47 episodes per 1000 patients-day, with 73% corresponding to primary bacteremias and CRB.67 In contrast, Buetti et al., in their case-COntrol study, found that COVID-19 patients have no greater risk of CRB than non-COVID-19 patients.68 Both studies do coincide in describing a greater risk of CRB in patients treated with corticosteroids, tocilizumab or anakinra – observations that could not be confirmed in the clinical trials with these drugs.
The situations in which CRB should be suspected, and the required diagnostic procedures, are no different from those referred to non-COVD-19 patients.69 With regard to management, there is no evidence to establish treatment regimens different from the usual ones – though some aspects need to be considered. In relation to the choice of antimicrobial therapy and catheter withdrawal, patients treated with corticosteroids or tocilizumab are to be regarded as immunosuppressed individuals, at least during treatment with corticosteroids and between two and four weeks after the administration of tocilizumab. We should adapt the antimicrobial treatment to the local resistances profile, focusing special attention on the changes in microbiology that might appear derived from the peculiarities of COVID-19 patients (Table 3), the high frequency of treatment with cephalosporins upon admission, and care of critical patients in areas different from the usual areas.
Device-related urinary tract infectionAccording to the data of the ENVIN-HELICS report of the year 2020,5 which describe the analysis of 1525 patients with SARS-CoV-2 pneumonia in the first wave of the pandemic, 19% of the infections related to medical care corresponded to bladder catheter-related urinary tract infections (C-UTI), with an incidence of 6.54 C-UTI episodes per 1000 days of catheter. A series of factors may predispose to the development of C-UTI, particularly a prolonged ICU stay, immune alterations, the need for an indwelling bladder catheter, and antibiotic treatment. The strategy for the prevention of C-UTI in the ICU has been extensively developed in the UTI-ZERO Project,70 and there are no differential aspects applicable to patients with SARS-CoV-2 infection. The most frequently isolated organism has been Enterococcus faecalis (Table 3). The change in microbiology observed in C-UTI in patients with SARS-CoV-2 pneumonia must be interpreted with caution, since it may be explained by the initial management approach involving cephalosporins, which since then has changed. Accordingly, until new data are forthcoming, the antibiotic treatment of these patients should ensure the coverage of gramnegative bacilli, considering the significant percentage of P. aeruginosa isolates. Antifungal treatment can be provided by fluconazole in patients with symptomatic candiduria and in those with asymptomatic candiduria and a risk of disseminated disease, as in neutropenic individuals, immunosuppressed patients or patients subjected to urological manipulations. In the case of infection due to Candida krusei or Candida glabrata resistant to azoles, use can be made of amphotericin B deoxycholate via the intravenous route. The echinocandins have been shown to be effective in some cases despite their scant elimination in urine. The current tendency in relation to the duration of treatment is to prescribe short cycles of between 3–7 dias.71,72
Opportunistic infections with special emphasis on invasive fungal infectionIn its more severe presentations, pneumonia due to SARS-CoV-2 has been associated with an increase in the incidence of opportunistic infections. Although a prolonged ICU stay or treatments with corticosteroids and/or immune modulators can be identified as risk factors in these patients, there is growing evidence that infection due to this virus and the development of ARDS give rise to lymphocyte dysfunction,73 which in turn can favor the development of opportunistic infections. We will focus on the two most common opportunistic infections in patients with COVID-19: invasive pulmonary aspergillosis and the reactivation of Herpesviridae. A marked increase in Candida spp. isolates has been observed, though the treatment in such cases is no different from that indicated in patients without SARS-CoV-2 infection.
Pulmonary aspergillosis associated to SARS-CoV-2 infectionPulmonary aspergillosis is a feared complication, due to its high associated mortality rate in critical patients subjected to mechanical ventilation. On occasion of the influenza A H1N1 pandemic in 2009, a number of authors had described an increase in the incidence of pulmonary aspergillosis among patients that developed ARDS.74 This same situation has been documented in patients with severe pneumonia due to SARS-CoV-275,76; the latter condition therefore must be included as a risk factor, in which active assessment of aspergillosis is advised.
Clinical and radiological criteria may be of help in diagnosing this complication, though they lack the necessary specificity to establish the diagnosis on their own.77,78 The difficulties in detecting pulmonary aspergillosis has led to urgency in establishing specific diagnostic recommendations for patients with SARS-CoV-2.79,80 In this respect, and as a first measure, these patients should be considered to be at risk, and an active assessment of Aspergillus should be made, with the obtainment of respiratory samples – since the determination of galactomannan in the serum of non-neutropenic patients offers only low sensitivity. Sampling preferably should be invasive in the form of fiber bronchoscopy in order to better differentiate between colonization and infection. The microbiology laboratory should perform staining with calcofluor and/or KOH in search of the presence of fungal elements in the direct sample, with the quantitative determination of galactomannan, and culture. The SARS-CoV-2 pandemic is generating an important work burden, and the quantification of galactomannan antigen is not available every day of the week. Furthermore, the results referred to fungal growth in culture may take some time, and we therefore need to consider the use of other faster techniques with adequate sensitivity such as lateral flow assay (LFA), which provides clinicians with very valuable information for the early start of antifungal treatment.81 Other diagnostic procedures such as determination of the fungus using polymerase chain reaction (PCR) techniques, mass spectrometry or urine antigen determination are currently not available in most laboratories, though in future they undoubtedly can make a valuable contribution to the diagnosis of the disease.82Table 6 describes the recommendations for the management of aspergillosis in critical patients with SARS-CoV-2 pneumonia. These recommendations are in line with those established in the critical care setting regardless of whether SARS-CoV-2 pneumonia is present or not. Voriconazole and isavuconazole are considered to be the first line treatment options,83 though isavuconazole has a better safety profile in critical patients that tend to develop complications such as renal or liver dysfunction. On the other hand, the adequate use of voriconazole requires monitoring of its plasma levels. Amphotericin B in lipidic formulation is a possible option in view of the growing increase in strains resistant to azole drugs in Spain.84 Recently, the ECMM/ISHAM guidelines have recommended such treatment with amphotericin B, or the possibility of combination therapy with azoles and an echinocandin in cases characterized by resistance to azoles.85
Recommendations for the management of pulmonary aspergillosis in critical patients with SARS-CoV-2 pneumonia.
| 1. Consider all patients with severe SARS-CoV-2 pneumonia to be at risk of suffering pulmonary aspergillosis |
| 2. Conduct active assessment of aspergillosis, collecting preferably invasive respiratory samples via fiber bronchoscopy |
| 3. Evaluate the presence of the following diagnostic criteria, and if they are confirmed, start early antifungal treatment: |
| - Clinical criteria: fever and/or worsening of respiratory function determined by the PaO2/FiO2 ratio, and not attributable to other causes |
| - Radiological criteria: presence of a infiltrates on the plain chest radiographs |
| - Microbiological criteria (any of which justify the start of treatment): |
| Detection of galactomannan levels in respiratory sample >0.5 |
| Positive real-time PCR testing/lateral flow assay (LFA)* |
| Direct visualization of fungal elements, hyphae, in the respiratory sample (calcofluor stain) |
| Growth of Aspergillus spp. in culture |
The key to combating the high mortality rate described in critical patients with pulmonary aspergillosis is the early start of treatment, and in this regard it is essential to recognize SARS-CoV-2 as representing a risk scenario where early and active assessment of this infectious complication is needed.
Reactivation of Herpesviridae in critical patients with COVID-19The Herpesviridae family comprises several viruses, of which herpes simplex virus (HSV) and cytomegalovirus (CMV) will be addressed in this review. These viruses can remain in a latent state after primary infection, and can reactivate at a later stage if the conditions become favorable. The possibility of HSV or CMV systemic infection or infection confined to a given organ in the immune competent critical patient is the subject of intense debate. Some authors consider that the detection (using quantitative or qualitative PCR) of the presence of the virus should not be regarded as an indication of treatment, since not all studies have demonstrated benefits of such treatment in terms of patient mortality.86 Nevertheless, a recent meta-analysis has concluded that treatment with acyclovir reduces in-hospital mortality and mortality at 30 days.87 Factors such as a high number of viral copies, a lack of response to antibiotic treatment, or the presence of positive cytological data in the bronchoalveolar lavage (BAL) support the existence of pneumonia due to HSV and thus the start of treatment.88,89
In the case of COVID-19 patients, there is growing evidence of a high frequency of reactivation of HSV and CMV.90,91 Here again, interpretation of the results may prove complex. Nevertheless, given the relative immunosuppression state caused by the lymphopenia and medication use, and the publication of clinical cases that histologically demonstrate deep tissue involvement,92,93 early therapy should be considered.
The microbiological diagnosis, preferably based on quantitative PCR testing, should be considered in all patients with respiratory worsening and/or an infectious process – particularly when a bacterial origin is ruled out or the patient fails to respond to antibiotic treatment.88,89 Invasive sampling is advised (BAL or minilavage). The serological study of HSV and CMV and the quantification of CMV in plasma may be of help in evaluating the case.
The treatment of HSV infection is based on acyclovir. Gancyclovir is the drug of choice for CMV, though the presence of resistances or a lack of response may require the use of foscarnet.
Final considerationsThe main limitation of this document is that the recommendations made are not fundamented upon any analysis of the evidence, since at this time there is still much to be learned about how the pandemic should be managed, and very few studies with an adequate methodological design have been able to contribute solid information in this respect. The existing evidence therefore must be classified as being of low level. Nevertheless, it can be concluded that the scarce evidence on effective treatments applicable to SARS-CoV-2 viral infection in critical patients focuses on supportive measures, the prevention of infections related to medical care, and the early detection and treatment of those infectious complications that have been described as being common in these patients.
Authors/collaboratorsAll the authors form part of the GTEIS of the SEMICYUC, and were selected by its coordinators for development of the present document.
They have participated in the preparation of all the document sections and have approved the final version. AE and RZ coordinated the project that gave rise to this document.
Conflicts of interestAE have participated in speeches/training activities organized by Pfizer, Gilead, MSD.
PVC has participated in speeches/training activities organized by Pfizer, Shionoghi, MSD.
RZ has participated in speeches/training activities organized by Pfizer, Shionoghi, MSD, Gilead.
The rest of the authors declare that they have no conflicts of interest.
Please cite this article as: Estella Á, Vidal-Cortés P, Rodríguez A, Andaluz Ojeda D, Martín-Loeches I, Díaz E, et al. Manejo de las complicaciones infecciosas asociadas con la infección por coronavirus en pacientes graves ingresados en UCI. Med Intensiva. 2021;45:485–500.