To describe changes in pulmonary mechanics when changing from supine position (SP) to prone position (PP) in mechanically ventilated (MV) patients with Acute Respiratory Distress Syndrome (ARDS) due to severe COVID-19.
DesignRetrospective cohort.
SettingIntensive Care Unit of the National Institute of Respiratory Diseases (Mexico City).
PatientsCOVID-19 patients on MV due to ARDS, with criteria for PP.
InterventionMeasurement of pulmonary mechanics in patients on SP to PP, using esophageal manometry.
Main variables of interestChanges in lung and thoracic wall mechanics in SP and PP
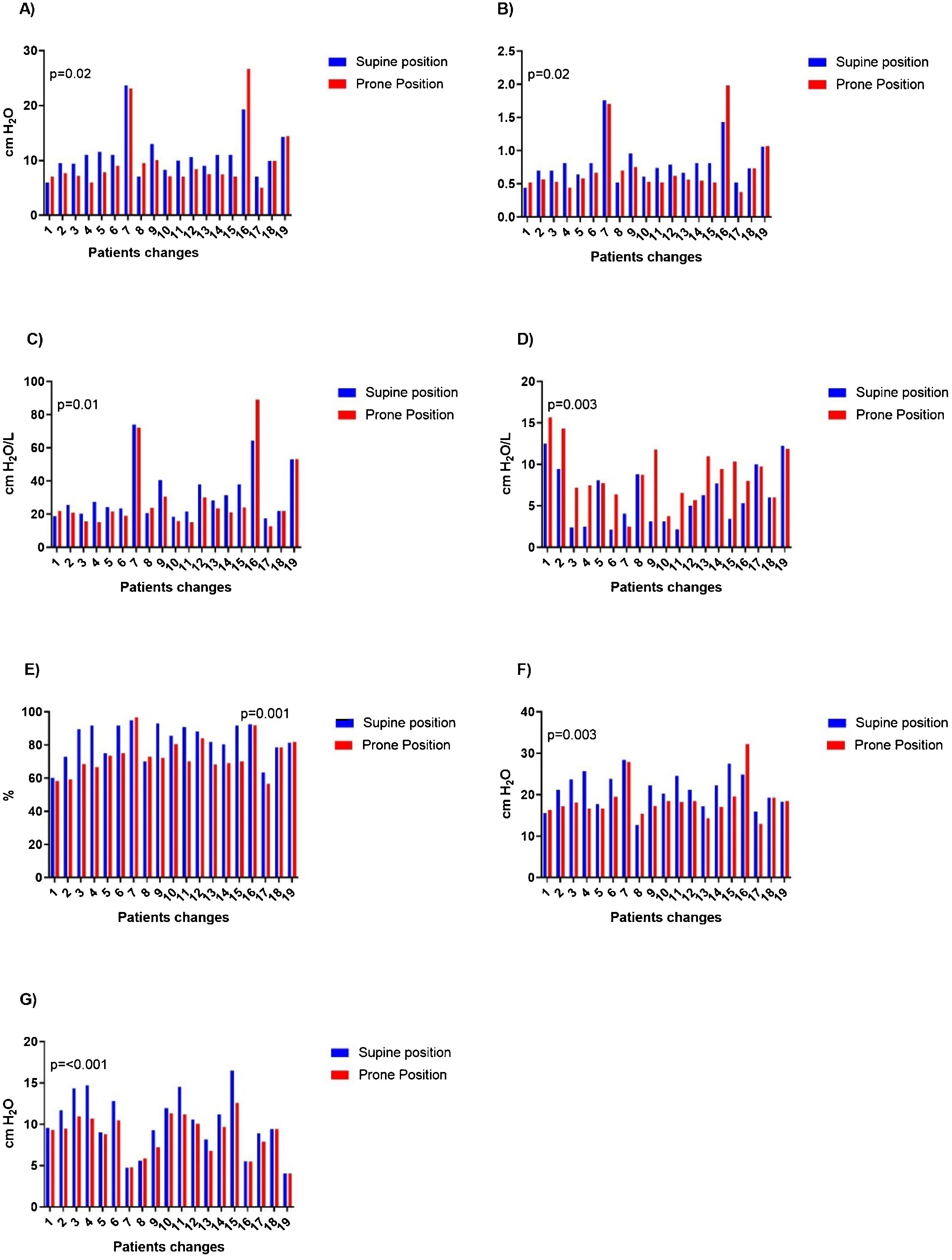
ResultsNineteen patients were included. Changes during first prone positioning were reported. Reductions in lung stress (10.6 vs 7.7, p=0.02), lung strain (0.74 vs 0.57, p=0.02), lung elastance (p=0.01), chest wall elastance (p=0.003) and relation of respiratory system elastances (p=0.001) were observed between patients when changing from SP to PP. No differences were observed in driving pressure (p=0.19) and transpulmonary pressure during inspiration (p=0.70).
ConclusionsChanges in pulmonary mechanics were observed when patients were comparing values of supine position with measurements obtained 24h after prone positioning. Esophageal pressure monitoring may facilitate ventilator management despite patient positioning.
Describir los cambios en la mecánica pulmonar de posición supino (SP) a posición prono (PP) en pacientes con ventilación mecánica (VM) con Sindrome de Insuficiencia Respiratoria Agudo Severo (SDRA) por COVID-19.
DiseñoCohorte retrospective.
ÁmbitoUnidad de Cuidados Intensivos Respiratorios del Instituto Nacional de Enfermedades Respiratorias, Ciudad de México.
PacientesSe incluyeron un total de 19 pacientes con criterios para PP.
Intervencionesmedición de la mecánica pulmonar en pacientes de SP a PP utilizando manometría esofágica.
Variables de interés principalesCambios en la mecanica pulmonar y de la pared torácica, medidas mediante manometría esofágica de posición supino a posición prono.
ResultadosSe observó una disminución en los valores medidos de estrés pulmonar (10,6 vs 7,7, p=0,02), “strain” pulmonar (0,74 vs 0,57, p=0,02), elastancia pulmonar (p=0,01), elastancia de la pared torácica (p=0,003) y en la relación de las elastancias del sistema respiratorio (p=0,001) tras el cambio de SP a PP. No se encontraron diferencias en la presión de conducción (p=0,19) ni en la presión transpulmonar durante la inspiración.
ConclusionesSe observaron cambios en la mecánica pulmonar al comparar los valores en posición supino y los medidos 24horas posteriores a la posición prono. El monitoreo de la presión esofágica puede ser de utilidad para el manejo del ventilador independientemente e la posición del paciente.
Acute Respiratory Distress Syndrome (ARDS) has been a common condition in Intensive Care Units.1 Severe ARDS cases increased during coronavirus disease (COVID-19) pandemic and were associated with higher rates of mortality in patients with mechanical ventilation (MV); this situation remarks the importance of appropriate ventilatory strategies for adequate tissue oxygenation.2
Prone positioning (PP) can improve oxygenation through a more homogeneous distribution of alveolar ventilation towards the dependent regions, with a reduction of the applied tension and stress to the lung parenchyma. When used at the early stage of the disease with prolonged sessions, PP has shown to reduce ventilator – induced lung injury and mortality.3–5 Reports suggests that longer time in the prone position, gives more benefit.5 Even when PP is not exempt from complications (dislodging endotracheal tube, removal of arterial or venous catheters, pressure sores, brachial plexus injury and hemodynamic instability),6 there are reports of continuous prone without interruptions of up to 9 days with minimal complications.7
Esophageal pressure (Pes) is used as a surrogate of pleural pressure (Ppl) at bedside on critically ill patients and there is evidence of improvements on oxygenation and compliance when it is used for adjustment of the settings of mechanical ventilation.8 The transpulmonary pressure (PL), one of the possible clinical applications of Pes9; is calculated as the difference between the airway pressure (Paw) and Ppl, separating the lung distending pressure from the applied pressure over the chest wall. For this reason, it has been proposed to set a positive end-expiratory pressure (PEEP) in order to maintain a PL positive value.10 PL might also be estimated from the airway plateau pressure (Pplat) and the relation between lung elastance (EL) and respiratory system elastance (ERS). Some data suggest that this EL derived method might be better to determine PL in nondependent lung regions, with a higher risk of hyperinflation. PL derived from the end-inspiratory EL might be a good substitute for lung stress.10
Even when Pes precision to estimate Ppl has been previously evaluated in ARDS patients at supine position, there are no reports during prone position. The aim of this study was to describe the pulmonary mechanics differences when changing from SP to PP in critically ill patients with severe ARDS due to COVID-19 infection.
MethodsThis was a retrospective cohort study of consecutive critically ill patients (>18 years) that were admitted to the Intensive Care Unit of the National Institute of Respiratory Diseases in Mexico City, from March 2021 to December 2021. COVID-19 patients (confirmed by SARS-CoV2 Real-time Polymerase Chain Reaction) on MV due to ARDS, with criteria for PP during first 24h were included. Only patients who had an indication for PP in accordance with our department’s protocol (PaO2/FiO2 ratio of <150mm Hg and FiO2 of ≥0.6 with PEEP of at least 5cm H2O) were considered eligible for the study.
According to our unit standard, PP was achieved with foam wedges and pillows, alternating head, and neck rotation every 4h. Duration of PP cycle is continuous (24h) without cycles SP changed.
Patients were excluded if it was necessary to modify the configuration of ventilatory parameters when changing to PP. This study had institutional review board approval (#C49-21), and informed consent was waived.
Data collectionDemographic data (gender, age and BMI) were obtained from medical records. Disease severity scales such as Sequential Organ Failure Assessment (SOFA) and Acute Physiology and Chronic Health Disease Classification System II (APACHE II) were calculated upon admission. Mortality were registered.
Pulmonary mechanics and transpulmonary pressure monitoringA 5 French catheter with an esophageal balloon (Cooper Surgical, Trumbull, Connecticut), was placed in the first 24h of mechanical ventilation, through the mouth with the patient in SP with a 30° bed angle. Catheter was placed in the esophagus according to esophageal catheter insertion procedure previously described.11 Position was confirmed with an expiratory airway occlusion maneuver with chest compression, recording the changes in esophageal and airways pressures. An adequate position was considered when the relation between esophageal pressure and the change in airways pressure ranged from 0.8 to 1.2 during occlusion maneuver. Visualization of the cardiac artifact on the esophageal pressure waveform was also used to qualitatively confirm proper catheter position. Esophageal pressure and LP graphs were monitored through the interface of the Hamilton S1 or C6 mechanical ventilation equipment (Hamilton Medical AG, Bonaduz, Switzerland) at the time of PEEP titration (time 0 in supine position) and 24h later to the maneuver (T2). Mechanical ventilation settings were adjusted to target an inspiratory PL<20cm H2O and an expiratory PL target of 0–6 H2O.
Pulmonary mechanics (Static compliance, driving pressure, lung stress and strain, EL, chest wall elastance, relation of ERS (lung/chest wall elastances), transpulmonary pressure during inspiration and expiration and inspiratory and expiratory EL-derived PL) were measured before PP and 24h after positioning during the first PP of each patient.
Statistical analysisData were analyzed using Stata Intercooled (Version 14, STATA Corporation, College Station, TX, USA) and GraphPad Prism (GraphPad Software Inc., San Diego, USA. The normality of the distribution of quantitative variables was verified by the Shapiro Wilk test. Descriptive statistics were used for the analysis of categorical variables (absolute and relative frequency) and quantitative variables (mean and standard deviation (SD) or median and interquartile range (IQR)). Clinical data were compared using the paired Student’s t-test or Wilcoxon test. Statistical significance was defined as p<0.05.
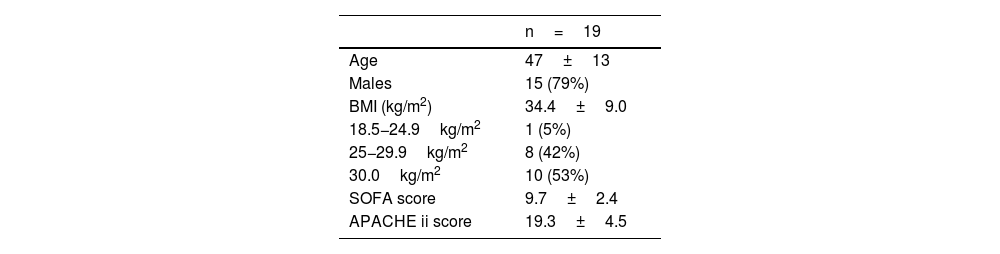
ResultsNineteen patients were included, of these 15 (79%) were male. Mean BMI was 34.4±9.0kg/m2, when categorizing the patients, 10 (53%) were obese (BMI>30kg/m2) and 8 (42%) were overweight. Mean age was 47±13 years, of which 3 patients (15%) were older than 60 years. Disease severity upon admission to the ICU was assessed with the SOFA scale presenting a mean of 9.7±2.4 points, and an APACHE II score of 19.3±4.5 points (Table 1). A total of 9 patients (47%) died during hospital stay.
When evaluating the changes in the ventilatory parameters when positioned from SP to PP, an increase in static compliance from 29.9±9.7 to 31.9±11.3ml/cm H2O (p=0.58) was observed. Mechanics ventilatory parameters are summarized in Table 2.
Pulmonary mechanics in critically-ill patients with COVID-19 when changing from SP to PP.
| Parameter | Supine | Prone | P value |
|---|---|---|---|
| Static compliance, ml/cm H2O | 29.9±9.7 | 31.9±11.3 | 0.58b |
| Driving pressure, cm H2O | 12 (11−13.7) | 11 (10−13) | 0.19a |
| Lung stress, cm H2O | 10.6 (9−11.6) | 7.7 (7−9.9) | 0.02a |
| Lung strain | 0.74 (0.64−0.81) | 0.57 (0.52−0.73) | 0.02a |
| Lung elastance, cm H2O/L | 25.6 (20.6−37.9) | 21.8 (15.8−30) | 0.01a |
| Chest wall elastance, cm H2O/L | 5.3 (3.1−8.8) | 8 (6.3−10.9) | 0.003a |
| Relation of respiratory system elastances (lung/chest wall elastances), cm H2O/L | 85.5 (75−91.6) | 72.1 (68.1−80.6) | 0.001a |
| Transpulmonary pressure during inspiration, cm H2O | 12.6±3.1 | 13±4.4 | 0.70b |
| Transpulmonary pressure during expiration, cm H2O | 3 (-2 - +4.6) | 3 (1.5−4.6) | 0.19a |
| Inspiratory elastance-derived transpulmonary pressure, cm H2O | 21.1±4.2 | 18.6±4.4 | 0.01b |
| Expiratory elastance-derived transpulmonary pressure, cm H2O | 10.1±3.5 | 8.7±2.4 | 0.0006b |
Reductions in lung stress (10.6 vs 7.7, p=0.02) and lung strain (0.74 vs 0.57, p=0.02), EL (p=0.01), chest wall elastance (p=0.003) and relation of ERS (p=0.001) were observed when changing from SP to PP. (See Fig. 1).
DiscussionThis study describes the changes in lung and thoracic wall mechanics measured by esophageal manometry in severe ARDS due to COVID-19. Knowledge of lung mechanics measured by esophageal manometry when changing from SP to PP, allows to understand at bedside how pulmonary physiology is maintained during critical illness; also offering the possibility to identify which variables could be implied in lung protection.
Our results showed a reduction in EL of the chest wall, which implies a greater rigidity explainable by the solidity of the sternum, associated with a significant decrease in pulmonary EL, tension stress and strain, which can be explained by a more homogeneous distribution of tidal volume and transpulmonary pressures.12
In our study, esophageal pressure was not significantly different when changing from SP to PP, even considering the modification in mediastinum configuration with the change in positioning. This observation which is similar to Aguirre-Bermeo et al.13 results, lead us to consider viability of these measures in patients with severe ARDS independently of position.
When changing from SP to PP, breastbone movement turns limited leading the chest to move between two rigid surfaces, which results in a homogeneous tidal volume distribution and a lower risk of lung injury. This is why PP is considered as a lung protection maneuver by itself. Similar to Riad et al.14 results, an increased elastance of the chest wall was observed when our patients were placed at prone position. However, we observed a reduction in EL during PP, which differs from the studied by Riad et al; where EL measures maintained the same values. This observation in our study might be explained by the homogeneous distribution of tidal volume that was previously described in PP, as a protective factor against lung injury.
When evaluating lung stress in our study, it was significantly reduced when changing from SP to PP. This finding which is similar to Mentzepoulos et al.15 observations allows us to stablish again the lower risk of ventilation-induced lung injury associated to PP, regardless of the fact that the driving pressure did not change significantly. Being the driving pressure one of the most relevant lung protection parameters in the present, we must consider that it depends of various factors such as the relation between lung elastance and chest elastance, when the latter one decreases as in our study; lung stress is reduced even when driving pressure remains the same or shows minimal changes.
Lung stress increased in 5 (26.3%) patients when changed from SP to PP, increasing the risk of lung injury and may be explained by other factors such age, other chronic diseases, and infection evolution. Considering this, we suggest the integral assessment of lung mechanics and not only the PP response by oxygenation for identify patients that may be beneficiated or prejudicated by this position.
In our sample, we observe a decrease in EL when changing the position of the patients from SP to PP, that can be explained by alveolar recruitment without changes in static compliance. Compliance differs between lung and the chest wall; however, the static compliance does not distinguish between them.16 The pressure applied to the lungs is the most important for the risk of lung injury, which could justify the importance of monitoring esophageal pressure when changing position from supine to prone and not just monitoring the static compliance.
The present study has limitations; (a) the results were obtained from a single center with a small sample size, that limits the study's ability to detect moderate to small changes in all variables, (b) high mortality rate was observed because patients not responding to the initial mechanical ventilation maneuvers, nor to the initial PEEP titration by esophageal manometry
ConclusionChanges in pulmonary mechanics were observed when patients were comparing values of SP with measurements obtained 24h after PP. Esophageal pressure monitoring may facilitate ventilator management despite patient positioning.
Authors' contributionsI. Maldonado-Beltrán, C.M. Hernández-Cárdenas, I.A. Osuna-Padilla, M.A. Ríos-Ayala, equally contributed to the conception, design of the research; I.A. Osuna-Padilla and I. Maldonado-Beltrán contributed to the analysis and interpretation of the data; N.C. Rodríguez-Moguel, C.M. Hernández-Cárdenas and G. Lugo-Goytia drafted the manuscript. All authors critically revised the manuscript, agree to be fully accountable for ensuring the integrity and accuracy of the work, and read and approved the final manuscript.
Conflictof interestAll authors declare that they have no conflict of interests
FundingThis research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
We gratefully acknowledge all of the physicians, nurses and dietitians for their dedication to the study.