To evaluate the diagnostic performance of FENa (Fractional excretion of sodium), FEK (fractional excretion of potassium) and uSID (urinary strong ion difference) in predicting pAKI in sepsis and septic shock.
DesignRetrospective cohort study.
SettingTwo intensive care units in Argentina.
PatientsAdult patients with a confirmed diagnosis of sepsis or septic shock and AKI, and had a urinary biochemistry within 24h of the AKI diagnosis.
InterventionsNone.
Main variables of interestWe evaluated the diagnostic accuracy of FENa, FEK and uSID through a ROC (Receiver Operating Characteristic) curve analysis.
Results80 patients were included. 40 patients presented pAKI. pAKI group had higher APACHE, SOFA score, and mortality rate. In the ROC curve analysis, uSID had no diagnostic utility (AUC=0.52, p=0.69). FENa presented moderate accuracy showing an AUC of 0.71 (95% CI 0.60−0.83; p=0.001), while FEK presented low accuracy with an AUC of 0.69 (95% CI 0.57−0.80; p=0.04). The optimal Youden point for identifying pAKI was at a FENa higher than 0.51 % with a specificity of 72.5% and a sensitivity of 65.0%. In the case of FEK, a value higher than 21.9 % presented the best relation, with a specificity of 67.5% and a sensitivity of 65.0%.
Conclusionsurine biochemistry interpretation in septic patients must be revised. FENa and FEK are related to the severity of AKI and could be helpful complementary tools for diagnosing pAKI.
Evaluar la utilidad diagnóstica de la Excreción fraccional de Sodio (FENa), Excreción fraccional de potasio (FEK) y uSID (diferencia de aniones fuertes urinaria) en el diagnóstico de la IRA persistente (IRAp).
Ámbito2 unidades de cuidados intensivos en Argentina.
PacientesAdultos con diagnóstico de sepsis o shock séptico e injuria renal aguda (IRA) y disponibilidad de una bioquímica urinaria dentro de las 24hs del diagnóstico de la IRA.
IntervenciónNinguna.
Variables de interés principalesEvaluamos la capacidad diagnóstica de la FENa y FEK y la brecha aniónica urinaria mediante un análisis de la curva ROC (Receiver Operating Characteristic).
ResultadosSe incluyeron 40 pacientes en cada grupo (IRAp vs transitoria). Los pacientes con IRAp tuvieron mayor APACHE, SOFA y mortalidad. En el análisis de las curvas ROC, la uSID no demostró utilidad diagnóstica (AUC=0.52). La FENa presentó moderada precisión con un AUC de 0.71 (IC95% 0.60–0.83), mientras que la FEK tuvo un AUC de 0.69 (IC95% 0.57−0.80). El punto de Youden para diferenciar IRAp para la FENa fue de 0.51% con una sensibilidad de 65.0% y una especificidad de 72.5%. En el caso de la FEK, el punto óptimo fue de 21.9% con una sensibilidad de 65.0% y una especificidad de 67.5%.
ConclusionesLa interpretación de la bioquímica urinaria en pacientes sépticos debe ser revisada. La FENa y FEK están relacionados con la severidad de la IRA y pueden ser herramientas diagnósticas complementarias de utilidad.
Acute Kidney Injury (AKI) is a common complication for patients admitted to the intensive care unit (ICU).1 Among its causes, sepsis-associated AKI (S-AKI) is the most frequent, accounting for 50% of cases.2 The pathophysiology of S-AKI is still poorly understood. The absence of characteristic histopathologic findings suggests that it could be a functional phenomenon, at least in the initial stages.3,4 Despite its limitations, AKI diagnosis and staging are based both on diuresis and serum creatinine values.5 Following the last consensus guidelines, persistent (pAKI) and transient AKI (tAKI) are defined as an AKI episode lasting more or less than 48−72h, respectively.6 Among them, pAKI might have a bigger impact on patient survival.7
The use of urine biochemistry and indices for guiding therapeutics presents multiple limitations. Fractional excretion of sodium (FENa) was originally conceived to be used on dehydrated patients and applying it in the context of sepsis may be misleading. Recent studies have shown that septic patients exhibit a low FENa when AKI develops, reflecting hyperactivation of the renin-angiotensin-aldosterone system (RAAS) and microcirculatory stress.8 Therefore, a FENa lower than 1% does not necessarily represent a hypovolemic state in septic patients, as it is essentially a constant variant.9
Alternative parameters have been explored, including Fractional excretion of potassium (FEK) and urinary strong ion difference (uSID).10,11 Elevated SIDu, in the presence of metabolic acidosis, might reflect the kidney’s inability to acidify urine (less tubular ammonia secretion). Thus, “intrinsic” damage may be manifested this way at the tubular level.10 Additionally, high FEK values reflect RAAS hyperactivation during early AKI and kidney stress. In this regard, both uSID and FEK may be valuable tools for detecting early physiologic disruptions, as well as predicting pAKI.
Given this background, the main objective of this study was to evaluate sensitivity, specificity, and under the ROC curve of FENa, FEK and uSID in a specific population of S-AKI patients, employing the latest consensus definitions. Additionally, we aimed to ratify previous findings regarding these indices.
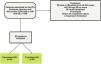
Patients and methodsStudy designWe conducted a retrospective cohort study including adult patients with S-AKI admitted to the ICU from January to December of 2019, at the Hospital Italiano de Buenos Aires and Hospital Italiano de San Justo, two tertiary teaching hospitals located in Argentina. Patients were eligible if they were 18 years or older, had a confirmed diagnosis of sepsis or septic shock and AKI,5 had a urinary biochemistry within 24h of the AKI diagnosis and creatinine values for at least five days. Patients with a history of chronic kidney disease stage 3b or worse, renal transplant recipients, cirrhosis and obstructive AKI were excluded (Fig. 1). Individuals were screened consecutively, from January 2019, and stopped when both groups had the necessary number of patients for the ROC (Receiver operating characteristic) analysis. Follow-up was performed from AKI diagnosis until hospital discharge or death.
This study was approved by the local ethics review board (protocol number 5655) and was conducted according to the amended Declaration of Helsinki. The protocol followed the “Standards for Reporting Diagnostic Accuracy Studies” (STARD) guidelines.
Study definitionsAKI was defined following the 2012 Kidney Disease: Improving Global Outcomes (KDIGO) definitions.5 Baseline creatinine was defined as the last creatinine obtained in the ambulatory setting within the last year before hospital admission and the estimated glomerular filtration rate was calculated using the CKD-EPI formula.12 Transient AKI was defined as an episode lasting less than 72h from onset with sustained reversal for at least 48h, and persistent AKI as an episode lasting more than 72h. Acute kidney disease (AKD) was defined as a patient meeting KDIGO criteria for AKI for at least seven days from onset.6 S-AKI was defined as an AKI episode occurring in patients with a diagnosis of sepsis or septic shock following the sepsis-3 consensus.13 Acute Physiology and Chronic Health Evaluation II (APACHE II) and Sequential Organ Failure Assessment (SOFA) scores were used for assessing disease severity and organ failure.14 The requirement of renal replacement therapy (RRT) during hospital stay was also recorded.
Urinary parameters obtained within 24h of AKI diagnosis were calculated as follows:
- -
Fractional excretion of potassium (FEK+) (%)=[(UK+(mEq/l)/K+(mEq/l))/(UCr (mg/dl)/SCr (mg/dl))] × 100.
- -
Fractional excretion of sodium (FENa+) %=[(UNa+(mEq/l)/Na+(mEq/l))/(UCr (mg/dl)/SCr (mg/dl))] × 100.
- -
Urinary strong ion difference (uSID): UNa+(mEq/l) + UK+(mEq/l) − UCl−(mEq/l)
- -
Demographics, comorbidities, Charlson comorbidity index,15 drugs from the ambulatory setting [e.g. immunosuppressants, chemotherapy, statins, diuretics, angiotensin-converting enzyme 2 inhibitors (ACEI) and Angiotensin Receptor Blocker (ARB)], nephrotoxic exposure (polymyxins, vancomycin, aminoglycosides and furosemide) and laboratory data from electronic health records were captured. In addition, a nephrologist and a critical care specialist (NCR) reviewed electronic medical charts to assess the cause of AKI. Finally, invasive mechanical ventilation (IMV) and vasopressor requirements, the length of hospital stay, and in-hospital mortality were recorded for each patient.
This study’s objective was to evaluate the diagnostic performance of FENa, FEK and uSID to diagnose persistent AKI in the septic population.
Statistical analysisContinuous variables were presented with mean and standard deviation (SD), or median and quartile ranges, and compared with T-Test, Wilcoxon according to distribution. Rate comparisons were performed by chi-squared test.
We performed a ROC analysis to determine the diagnostic performance of the different urinary indices. The sample size for this was calculated hypothesizing that the area under the curve (AUC) needed for discrimination between transient and persistent AKI was greater than 0.7; being the null hypothesis AUC=0.5; with an alpha and beta error of 0.05 and 0.10, respectively. Based on this, 40 patients in each group were needed. The Youden point was selected to define the best relation between specificity and sensitivity.
SPSS version 23 (IBM) was used for analysis and ROC plotting. MedCalc Version 20.305 was used for sample size calculation. All reported p-values are two-sided and p-value < 0.05 was used as the threshold for statistical significance.
ResultsA total of 199 patients with S-AKI diagnosis admitted to the ICU were initially evaluated. 119 patients were excluded (Fig. 1). The most frequent causes of exclusion were chronic kidney disease KDIGO stage 3b or higher and the lack of urinary biochemistry within the 24h of AKI diagnosis. Overall, 80 patients were finally included in the analysis.
Baseline clinical, demographic and laboratory data are presented in Table 1. The cohort comprised older adults (mean age 70.7 years old, SD 15.3) and 59.5 % were male. It is worth mentioning that hypertension and diabetes mellitus were the most prevalent comorbidities, 61.3 % and 17.5 %, respectively, with no difference between groups. Only 7 individuals (8.7%) had a baseline estimated glomerular filtration rate lower than 60ml/min and were more prevalent in the pAKI group (15%). No differences in regular medications received in the ambulatory setting were found.
Baseline characteristics of patients in the study.
| Baseline characteristic | Entire cohort (n=80) | Transient AKI(n=40) | Persistent AKI(n=40) | p-value |
|---|---|---|---|---|
| Demographic characteristics | ||||
| Age, years, mean (SD) | 70.7 (15.3) | 71.1 (14.16) | 70.2 (16.5) | 0.78 |
| Male sex, n (%) | 47 (59.5) | 23 (57.5) | 24 (61.5) | 0.71 |
| Length of hospital stay in days, median (IQR) | 15 (9−28) | 13 (8−23) | 16 (10−34) | 0.12 |
| Baseline comorbidities | ||||
| Charlson severity index, median (IQR) | 5.5 (4−7) | 5.5 (4−7) | 5 (3.5−7) | 0.87 |
| Diabetes mellitus, n (%) | 14 (17.5) | 6 (15.0) | 8 (20.0) | 0.57 |
| Hypertension, n (%) | 49 (61.3) | 23 (57.5) | 26 (65) | 0.49 |
| CKD-EPI less than 60ml/min, n (%) | 7 (8.7) | 1 (2.5) | 6 (15.0) | 0.04 |
| Malignancy, n (%) | 13 (16.5) | 9 (22.5) | 4 (10.3) | 0.14 |
| Regular medications in the ambulatory setting | ||||
| ACEI/ARB, n (%) | 33 (41.3) | 16 (40.0) | 17 (42.5) | 0.82 |
| Chemotherapy, n (%) | 13 (16.5) | 7 (17.5) | 6 (15.4) | 0.79 |
| Statins, n (%) | 21 (27.6) | 13 (32.5) | 8 (22.2) | 0.31 |
| Furosemide, n (%) | 7 (9.6) | 3 (7.5) | 4 (10.0) | 0.69 |
CKD-EPI: Chronic Kidney Disease Epidemiology Collaboration; ACEI: Angiotensin-converting enzyme inhibitor; ARB: Angiotensin receptor blocker.
The severity of illness in patients with pAKI was greater, reflected by higher APACHE and SOFA scores at ICU admission, IMV requirement and septic shock incidence. A roughly six-fold increase in the mortality rate during hospital stay among patients developing pAKI was observed. Overall, 9 subjects (11.5%) required RRT (Table 2).
Clinical and laboratory data of persistent and transient AKI episodes.
| AKI characteristics | Entire cohort (n=80) | Transient AKI(n=40) | Persistent AKI(n=40) | p-value |
|---|---|---|---|---|
| Laboratory findings on the day of AKI onset | ||||
| Serum Sodium (mg/dl), mean (SD) | 134.3 (6.5) | 133.3 (5.9) | 135.3 (6.9) | 0.17 |
| Serum Potassium (mg/dl), mean (SD) | 4.1 (0.7) | 4.0 (0.6) | 4.2 (0.8) | 0.36 |
| Serum Chloride (mg/dl), mean (SD) | 102.1 (8.0) | 100.6 (7.8) | 103.5 (8.0) | 0.10 |
| Serum Creatinine (mg/dl), mean (SD) | 2.1 (1.3) | 1.6 (0.5) | 2.5 (1.6) | 0.008 |
| Serum Urea (mg/dl), mean (SD) | 88.1 (45.7) | 74.2 (32.9) | 101.6 (51.4) | 0.008 |
| pH level, mean (SD) | 7.34 (0.08) | 7.37 (0.06) | 7.31 (0.08) | 0.003 |
| Base excess, mean (SD) | −3.3 (4.5) | −1.8 (3.5) | −4.8 (5.0) | 0.003 |
| Lactate (mmol/dl), mean (SD) | 2.7 (3.6) | 3.1 (5.0) | 2.4 (1.5) | 0.54 |
| UCr (mg/dl), mean (SD) | 103.9 (65.0) | 118.6 (77.1) | 89.3 (46.7) | 0.15 |
| UNa (mg/dl), mean (SD) | 37.0 (24.1) | 30.9 (20.3) | 43.2 (26.2) | 0.02 |
| UK (mg/dl), mean (SD) | 48.3 (25.0) | 51.3 (26.4) | 45.4 (23.4) | 0.29 |
| UCl (mg/dl), mean (SD) | 39.1 (25.8) | 37.3 (27.5) | 40.9 (24.2) | 0.53 |
| FENa (%), mean (SD) | 0.98 (1.5) | 0.5 (0.5) | 1.5 (2.0) | 0.001 |
| FEK (%), mean (SD) | 26.8 (19.0) | 20.3 (10.9) | 33.4 (22.8) | 0.003 |
| FECl (%), mean (SD) | 1.35 (2.3) | 0.7 (0.7) | 2.0 (3.0) | 0.01 |
| uSID, mean (SD) | 46.3 (27.6) | 44.9 (31.0) | 47.7 (24.0) | 0.64 |
| Urinary density, mean (SD) | 1019 (6.8) | 1020 (8.3) | 1019 (5.5) | 0.57 |
| Granulosus casts, n (%) | 17 (33.3) | 5 (20.8) | 12 (44.4) | 0.07 |
| Medications received on the day of AKI onset | ||||
| Vancomycin, n (%) | 30 (37.5) | 8 (20.0) | 22 (55.0) | 0.001 |
| Colistin, n (%) | 8 (10.0) | 0 | 8 (20.0) | 0.002 |
| NSAID, n (%) | 27(35.5) | 10 (27.8) | 17 (42.5) | 0.18 |
| Furosemide, n (%)a | 17 (21.3) | 6 (15.0) | 11 (27.5) | 0.17 |
| Diuresis and fluid balance | ||||
| 24-h diuresis on the day of AKi onset (l/24h), median (IQR) | 1.1 (0.7−1.9) | 1.0 (0.7−1.8) | 1.1 (0.6−1.9) | 0.82 |
| 48-h cumulative fluid balance (l/24h), median (IQR) | 2.7 (-1.7−4.7 | 0.3 (2.3−4.7) | 2.3 (1.5−4.6) | 0.36 |
| 72-h cumulative fluid balance, median (IQR) | −0,07 (−.1−2.2) | 0.7 (−2.4−2.2) | −0.6 (−2.1−1.9) | 0.56 |
| KDIGO staging | ||||
| Acute kidney disease, n (%) | 17 (27.0) | 0 | 17 (60.7) | <0.001 |
| RRT, n (%) | 9 (11.5) | – | 9 (22.5) | 0.002 |
| Stage of KDIGO the day of AKi onset (%) | ||||
| Stage 1 | 44 (55.0) | 27 (67.5) | 17 (42.5) | 0.03 |
| Stage 2 | 20 (25.0) | 11 (27.5) | 9 (22.5) | 0.61 |
| Stage 3 | 16 (20.0) | 2 (5.0) | 14 (35.0) | 0.001 |
| 72-h KDIGO stage, n (%) | ||||
| Stage 1 | 15 (18.75) | – | 15 (37.5) | – |
| Stage 2 | 9 (11.3) | – | 9 (22.5) | – |
| Stage 3 | 16 (20.0) | – | 16 (40.0) | – |
| Source of infection | ||||
| Pulmonary, n (%) | 29 (36.7) | 13 (32.5) | 17 (42.5) | 0.35 |
| Gastrointestinal, n (%) | 23 (29.1) | 12 (30.0) | 11 (27.5) | 0.85 |
| Urinary tract, n (%) | 13 (16.5) | 5 (12.5) | 8 (20.0) | 0.37 |
| Hepatobiliary, n (%) | 10 (12.7) | 9 (22.5) | 1 (2.5) | 0.007 |
| Skin and soft tissue, n (%) | 4 (5.0) | 1 (2.5) | 3 (7.5) | 0.31 |
| Severity of disease | ||||
| APACHE score the day of ICU admission, median (IQR) | 15 (11−20) | 14 (9.5−18) | 17 (12−28) | 0.02 |
| SOFA score on the day of ICU admission, median (IQR) | 6 (3−8) | 4.5 (3−6) | 6 (4−9) | 0.003 |
| Invasive mechanical ventilation, n (%) | 42 (53.2) | 14 (35.0) | 28 (71.8) | 0.001 |
| Shock, n (%) | 46 (58.2) | 17 (43.6) | 29 (72.5) | 0.009 |
| Mortality during hospitalization, n (%) | 15 (18.8) | 2 (5.0) | 13 (32.5) | 0.002 |
UCr: urinary creatinine; UNa: Urinary sodium; UK: Urinary potassium; UCl: urinary chloride; FENa: fractional excretion of sodium; FEK: fractional excretion of potassium; FECl: fractional excretion of chloride; uSID: urinary strong ion difference; NSAIDs: nonsteroidal anti-inflammatory drugs; RRT: renal replacement therapy; APACHE: Acute Physiology and Chronic Health Evaluation II; SOFA: Sequential Organ Failure Assessment; ICU: intensive care unit.
Regarding baseline biochemical parameters, individuals with pAKI presented lower pH and base excess values. On the other hand, they had higher plasma creatinine, urea, FENa and FEK. Of note, pAKI patients had higher exposure to nephrotoxic drugs such as vancomycin and colistin. No differences were found regarding 24-h or 72-h cumulative net fluid balance (Table 2).
The ROC analysis is presented in Fig. 2. uSID had no diagnostic utility (AUC=0.52, p=0.69). FENa presented moderate accuracy showing an AUC of 0.71 (95% CI 0.60−0.83; p=0.001), while FEK presented low accuracy with an AUC of 0.69 (95% CI 0.57−0.80; p=0.04). The optimal Youden point for identifying pAKI was at a FENa higher than 0.51 % with a specificity of 72.5% and a sensitivity of 65.0%. In the case of FEK, a value higher than 21.9 % presented the best relation, with a specificity of 67.5% and a sensitivity of 65.0%.
DiscussionThe main finding of our study was the fact that FENa and FEK presented moderate and low diagnostic accuracy for the discrimination between pAKI and tAKI in critically ill septic patients, respectively.16 However, we did not find a diagnostic utility for uSID in this setting.
FENa is a widespread tool for interpreting AKI used from the 70s due to the work of Espinel et al.17 However, the paradigm of prerenal and intrinsic AKI is under question. It is well known that patients with sepsis present a FENa <1% on the first days of AKI development.18 Also, in S-AKI, FENa is lower compared to other AKI etiologies. Based on these findings, different authors rejected FENa as a marker of pAKI in sepsis.19 In 2013, Vanmassenhove et al. in a prospective study, analyzed FENa and other biomarkers in 107 sepsis patients at admission. They found a lower value of FENa (0.36%) with a 92 % negative predictive value for intrinsic AKI or not restoring diuresis. They concluded that FENa values should be revised for this population. Our study aligns with this conclusion, with a FENa of 0.51 % representing the optimal Youden point. The AUC shows moderate accuracy for predicting pAKI,16 which is why our results must be interpreted carefully. Considering this limitation, this finding suggests that FENa still could be used as a complementary test for predicting pAKI in this setting, with a lower cut-off. It is an accessible tool for its availability in every ICU and has a lower cost than novel biomarkers.
In the last decade, Maciel et al. started to explore FEK as a diagnostic tool for pAKI.10,11 They considered it as fairly accurate for predicting pAKI, with an AUC of 0.71 (95% CI: 0.61−0.81; p<0.001) on the day of AKI diagnosis. A FEK of 18.3% was found to be the best cut-off value for discriminating pAKI, with a PPV of 69.3% and NPV of 72.6%. We confirmed these findings with similar values. FEK in this setting may be representing RAAS hyperactivation during sepsis. Medullary hypoxia produced by intrarenal shunt in sepsis may contribute to this, generating a loop diuretic effect due to Na-K-2Cl carrier dysfunction.20
Alterations in UCl are a part of AKI development.8 Kellum proposed that an adequate response to metabolic acidosis should be a negative uSID. During AKI, this mechanism could be damaged and would manifest as the renal incapability of Cl− excretion during metabolic acidosis, with a greater uSID.21 Balsonaro et al. showed in a retrospective cohort with sepsis, an excellent diagnostic performance for uSID on differentiating AKI from controls, while the AUC for distinguishing between pAKI and tAKI was more modest.10 We couldn’t reproduce this finding in our cohort. Two reasons may explain this. First, our patients did not present severe metabolic acidosis, although patients with pAKI were more acidotic. Second, we obtained data from the day of AKI diagnosis. In this early stage, urine acidification mechanisms may have not been activated yet.22
Some strengths must be noted. Firstly, we aimed to study a restricted sample of critical patients with S-AKI. Previous research has studied the general ICU population, including different causes of AKI, which makes it difficult for result interpretation. Secondly, we accurately determined the precise time frame in which AKI developed and when urinary biochemistry data was collected. The timing on which the urinary indices are performed is crucial to validate the diagnostic method for pAKI. Thirdly, we gathered information on factors associated with AKI, such as prior medications and nephrotoxic agents, on the day of AKI onset. Lastly, despite focusing on a S-AKI population, we employed a pragmatic approach and did not exclude patients with common confounders like exposure to nephrotoxic drugs, ACEI/ARBs, and diuretics. This approach enhances the applicability of our findings to clinicians managing patients in everyday practice.
Several limitations are present in this study. Although we studied a restricted population, there are factors other than sepsis that may be influencing kidney recovery in the pAKI group. Shock, nephrotoxic drugs and severity scores such as APACHE II and SOFA are higher in this group. Secondly, we couldn’t compare curves with novel biomarkers such as NGAL or KIM-1 because it is not routinely employed in our unit. Thirdly, the single-center nature of the study hinders the external validation of the study. On this line, factors regarding hemodynamic monitoring and fluid management may vary between centers and could be influencing renal outcomes.
Our data suggests that urine biochemistry utility in septic patients must be revised. FEK and FENa are related to AKI severity. In the setting of S-AKI, FENa and FEK could be helpful complementary tools for predicting pAKI on the day of AKI diagnosis.
Declaration of generative Artificial Intelligence (AI) and AI-assisted technologies in the writing processDuring the preparation of this work, the author did not use a generative AI tool in the writing process.
Conflict of interestThe authors declare no conflict of interest relevant to the content of this paper.