To evaluate head-of-bed elevation (HOBE) compliance in mechanically ventilated (MV) patients during different time periods, in order to identify factors that may influence compliance and to compare direct-observation compliance with checklist-reported compliance.
Design and settingA prospective observational study was carried out in a polyvalent Intensive Care Unit.
PatientsAll consecutive patients with MV and no contraindication for semi-recumbency were studied.
Intervention and variablesHOBE was observed during four periods of one month each for one year, the first period being blinded. HOBE was measured with an electronic device three times daily. Main variables were HOBE, type of airway device, type of bed, nursing shift, day of the week and checklist-reported compliance. No patient characteristics were collected.
ResultsDuring the four periods, 2639 observations were collected. Global HOBE compliance was 24.0%, and the median angle head-of-bed elevation (M-HOBE) was 24.0° (IQR 18.8–30.0). HOBE compliance and M-HOBE by periods were as follows: blinded period: 13.8% and 21.1° (IQR 16.3–24.4); period 1: 25.5% and 24.3° (IQR 18.8–30.2); period 2: 22.7% and 24.4° (IQR 18.9–29.6); and period 3: 31.4% and 26.7° (IQR 21.3–32.6) (p<0.001). An overestimation of 50–60% was found when comparing self-reported compliance using a checklist versus direct-observation compliance (p<0.001).
Multivariate logistic regression analysis found the presence of an endotracheal tube (ET) and bed without HOBE measuring device to be independently associated to greater compliance (p<0.05).
ConclusionsAlthough compliance increased significantly during the study period, it was still not optimal. Checklist-reported compliance significantly overestimated HOBE compliance. The presence of an ET and a bed without HOBE measuring device was associated to greater compliance.
Evaluar el cumplimiento de la elevación de la cabecera de la cama (ECC) en pacientes atendidos con ventilación mecánica (MV) durante distintos periodos de tiempo con el fin de identificar los factores que pueden influir sobre el cumplimiento y comparar el cumplimiento evaluado mediante observación directa con el cumplimiento evaluado mediante lista de verificación.
Diseño y ámbitoSe llevó a cabo un estudio observacional y prospectivo en una unidad de cuidados intensivos polivalente.
PacientesSe estudió a todos los pacientes consecutivos atendidos con MV y en los que no estaba contraindicada la reclinación parcial.
Intervención y variablesSe observó la ECC durante 4 periodos de un mes a lo largo de un año, el primero de ellos con enmascaramiento. Se midió la ECC mediante un dispositivo electrónico 3 veces al día. Las variables principales fueron ECC, tipo de dispositivo para las vías respiratorias, tipo de cama, turno de enfermería, día de la semana y cumplimiento notificado mediante lista de verificación. No se recopilaron las características de los pacientes.
ResultadosSe recopilaron 2.639 observaciones durante los 4 periodos. La tasa global de cumplimiento con la ECC fue del 24.0%, mientras que la mediana del ángulo de elevación de la cabecera de la cama (M-ECC) fue de 24.0° (IQR 18.8–30.0). El cumplimiento con la ECC y la M-ECC por cada periodo fue: periodo con enmascaramiento: 13.8% y 21.1° (IQR 16.3–24.4); periodo 1: 25.5% y 24.3° (IQR 18.8–30.2); periodo 2: 22.7% y 24.4° (IQR 18.9–29.6); y periodo 3: 31.4% y 26.7° (IQR 21.3–32.6) (p<0.001). Se observó una sobreestimación del 50–60% al comparar el cumplimiento autoevaluado por medio de una lista de verificación frente al cumplimiento evaluado mediante observación directa (p<0.001).
Un análisis de regresión logística multivariante concluyó que la presencia de un tubo endotraqueal (TE) y de una cama sin dispositivo de medición de ECC se asociaban de manera independiente a un mayor cumplimiento (p<0.05).
ConclusionesSi bien el cumplimiento aumentó de manera significativa durante el periodo del estudio, seguía sin ser el óptimo. El cumplimiento evaluado mediante lista de verificación sobreestimó de manera significativa el cumplimiento de la ECC. La presencia de un TE y una cama sin dispositivo de medición de ECC se asociaba a un mayor cumplimiento.
Semi-recumbent position is defined as head-of-bed elevation (HOBE) from 30 to 45°, and is recommended for the prevention of Ventilator-Associated Pneumonia (VAP) in all international guidelines.1–6 However, despite the broad recommendation of the use of HOBE for the prevention of VAP, evidence supporting this measure is limited.7–10
The first study supporting HOBE was published in 1992 by Torres et al.9 and reported that 45° HOBE significantly decreased the incidence of broncoaspiration when compared to supine position at 0°. Later, a randomized controlled trial comparing backrest patients positioned at 45° with patients positioned at 0° found a 76% decrease in VAP incidence in the 45° group.10 On the one hand, only these two randomized trials have prospectively demonstrated the effectiveness of HOBE at 45° for VAP prevention. On the other hand, other studies with more realistic control groups, such as HOBE of 25° or 10°, did not find any significant differences in VAP incidence compared to the 45° group.7,11 Regarding observational studies, a multivariate logistic regression analysis showed that keeping patients on at least 30° during the first 24h of mechanical ventilation (MV) was independently associated with lower VAP incidence and mortality.8 Due to lack of conclusive evidence supporting HOBE, the European Society of Intensive Care Medicine (ESICM) recommends elevating the head-of-bed from 20 to 45°, preferably >30°, unless it interferes with patient care or wishes.12
However, compliance is a factor that may limit the effectiveness of this recommendation. In fact, a common issue in all of the previously mentioned studies is low compliance10,11 or even non-report of compliance.7–9 For instance, in the study performed by Van Nieuwenhoven et al., the patients were positioned to 45° or 10° and compliance was monitored continuously. The investigators found that the group at 45° did not achieve this position for 85% of the time, being the median HOBE (M-HOBE) 28°.11 Studies particularly focusing on compliance have found that M-HOBE ranges from 19.2° to 28°13–15 and that HOBE compliance is below the optimal value, from 22.3% to 40.9%.15–18
Many strategies have been described that aim to increase compliance to HOBE, such as training sessions,16,19 devices to remind staff of the importance of the HOBE20 and even considering HOBE a clinical monitoring parameter.21,22 However, maintaining patients positioned at 30–45° still seems challenging.
Some studies evaluated the main factors associated with low compliance and concluded that airway device type, nursing shift, nursing experience, enteral nutrition, weaning and haemodynamic status of the patients were factors associated with low compliance.14,15,17,18
Most of the studies that evaluated HOBE compliance were performed during a 7-days period, regardless of whether they evaluated or not the relationship between HOBE and VAP.11,13,15,18,23 For the assessment of compliance during longer periods of time, self-reported checklists may be regarded as an alternative as they might be easier to implement compared to direct observation. Checklists have been demonstrated to be useful in improving adherence to patient's care24 and might have an impact in patient outcomes.25 However, the effectiveness of this measuring technique has not been yet evaluated for HOBE compliance. The aim of the present study was to assess the real HOBE compliance in a 14-bed Intensive Care Unit (ICU), to compare direct-observation with self-reported compliance using a daily checklist (checklist-reported) and to identify the factors that might influence HOBE compliance.
Patients and methodsA prospective, observational study was performed in a 14-bed polyvalent ICU, in a tertiary hospital. Study was undertaken from January 2012 to March 2013, during four time periods of one month in length each. HOBE was recorded from all patients requiring MV with no absolute contraindications for HOBE. Absolute contraindications for HOBE were pelvic fracture, suspected or confirmed spinal injury and anti-Trendelemburg and prone positioning. Study investigators registered HOBE three times daily (once per nursing shift), when the nurse was not in the patient room. For each nursing shift there were two study investigators responsible for data collection. The first evaluation period was over January 2012 [(Blinded period (BP)], where HOBE was audited without the awareness of the nursing staff in order to minimize the Hawthorne effect.26 To achieve this blinding, data were collected during the nurses’ break time. At the end of the BP, an intervention was implemented to all the health care workers. It consisted of presenting (1) the results of the BP evaluation, mainly median-HOBE (M-HOBE, (°) and HOBE compliance (%), and (2) the research project and the rationale for implementing HOBE. Afterwards, HOBE evaluation was continued using the methodology described above for another month [period 1 (P1)]. The follow-up observations were performed six and 12 months after BP, corresponding to P2 and P3 respectively.
Variables recorded for each measurement were: degrees of HOBE, airway device type (endotracheal tube (ET) or tracheostomy), type of bed (with or without HOBE measuring device), day of the week (weekday or weekend), nursing shift (day, evening or night) and checklist-reported compliance. The ICU has two types of beds, 7 beds with HOBE measuring device (Hill-Room Total Care®) and 7 beds without the device. The device available to measure the HOBE consists of a protractor with a small sphere inside. This bed has no alarm but the angle of elevation can be monitored continuously in an approximate manner.
Direct-observation compliance was defined as HOBE between 30.0° and 45.0°. Data were collected as observations rather than as individual patients.
The study investigators measured HOBE when patients were not undergoing clinical procedures in order to avoid position changes that may affect reliability of the data. HOBE was assessed at the mattress’ base of the bed, always using the same device (BOSCH GLM80®) regardless of bed type (Fig. 1). All the study investigators were properly trained by the principal investigator.
For comparing direct-observation with self-reported compliance, a checklist that included several VAP preventive measures was used, including HOBE between 30.0° and 45.0°. In the study unit, this checklist has been used routinely during three years before the onset of the study, and consists of 5 evidence-based interventions for VAP prevention, including HOBE. This checklist was completed at the end of every working shift. For each marked item, it was assumed that the intervention had been performed during the whole time period. In the present study, checklist-reported compliance was defined as whether or not the nurse marked in the checklist the accomplishment of HOBE recommendation during her working shift.
Ethical considerationsThe study was designed according to the ethical standards stated in the Helsinki Declaration and following the good clinical practices and it was approved by the local ethics committee. The informed consent was waived for all study subjects.
Data analysisStatistical analysis was performed using SPSS v15 for Windows (SPSS Inc., Chicago, USA). Results are expressed as absolute and relative frequencies for categorical variables and as medians with percentiles 25–75 (IQR 25–75) for continuous variables. U-Mann Whitney test was used for non-normally distributed variables, and Chi-square test was used for categorical variables. ANOVA analysis was performed to compare HOBE compliance across the four periods. A multivariate logistic regression model was developed in order to identify the factors independently associated with HOBE compliance. The variables were included in the multivariate analysis if they were significant in the univariate analysis (p<0.05). The logistic regression models were assessed for goodness of fit using the method of Hosmer and Lemeshow.27 The significance level for all the analyses was defined as p<0.05.
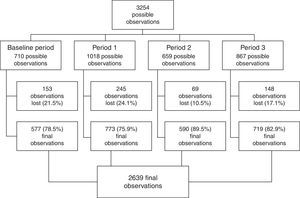
ResultsFrom a total of 3254 possible observations, 2639 observations were obtained (81.1%). Of these, 557 were obtained during BP, 773 during P1, 590 during P2 and 719 during P3 (Fig. 2). The remaining 18.9% observations were not obtained due to absence of study investigators or too high workload during some shifts.
Overall compliance was 24.0% with a M-HOBE of 24.0° (IQR 18.8–30.0). During the BP, M-HOBE was 21.1° (IQR 16.3°–25.4°) with a compliance of 13.8%. During P1 M-HOBE increased to 24.3° (IQR 18.8°–30.2°) (p<0.001), with a compliance of 25.5% (p<0.001). During P2 M-HOBE was 24.4° (IQR 18.9°–29.6°) and compliance was 22.7%. Finally, during P3 M-HOBE was 26.7° (IQR 21.3°–32.6°) with a compliance of 31.4%.
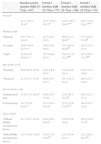
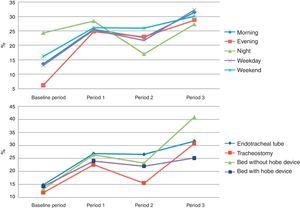
When comparing BP, P1, P2 and P3, significant differences were found among periods for M-HOBE and HOBE compliance, except for P1 versus P2. ANOVA showed statistical significance when comparing M-HOBE across the study periods (p<0.001) (Table 1 and Fig. 3).
M-HOBE during study periods, overall and by evaluated variables.
| Baseline period [median (IQR 25–75)]n=557 | Period 1 [median (IQR 25–75)]n=773 | Period 2 [median (IQR 25–75)]n=590 | Period 3 [median (IQR 25–75)]n=719 | |
|---|---|---|---|---|
| Overall | ||||
| 21.1° (16.3–25.4)α | 24.3° (18.8–30.2)αα | 24.4° (18.9–29.6) ααα | 26.7° (21.3–32.6) αααα | |
| Working shift | ||||
| Morning | 20.3° (15.3–24.4)* | 24.7 (19.1–30.2) | 26.6 (21.3–30.6)# | 27.7 (22.4–33.8)& |
| Evening | 20.6° (16.8–23.7)** | 24.6 (19.1–30.5) | 23.2 (18.4–28.8)## | 26.5 (21.4–32.3) |
| Night | 22.8 (17.0–30.0)*** | 23.5 (18.6–30.2) | 23.0 (17.5–28.3)### | 25.3 (20.1–31.5)&& |
| Day of the week | ||||
| Weekday | 20.8 (16.3–25.4) | 24.4 (18.8–30.2) | 24.4 (18.9–29.2) | 27.0 (21.2–32.6) |
| Weekend | 21.4 (15.3–27.4) | 24.0 (19.7–30.1) | 24.7 (19.1–30.2) | 26.0 (21.3–32.6) |
| Airway device type | ||||
| Endotracheal tube | 21.6 (17.5–26.8)+ | 24.8 (19.1–31.0)¿ | 25.6 (20.3–30.2)@ | 26.8 (21.2–32.7) |
| Tracheostomy | 18.7 (13.9–24.2)++ | 23.1 (18.3–29.3)¿¿ | 22.1 (17.8–27.6)@@ | 26.4 (21.5–32.4) |
| Type of bed | ||||
| Without HOBE measurement device | 21.7 (18.1–25.4)¡ | 24.8 (20.3–30.5)$ | 24.6 (19.9–29.9) | 29.2 (23.0–35.7)€ |
| With HOBE measurement device | 19.7 (14.6–25.6)¡¡ | 23.0 (17.8–30.0)$$ | 24.1 (18.4–29.2) | 25.2 (20.2–30.5)€€ |
Each symbol represents the M-HOBE of each period where significant differences were found compared to another one.αvsααp<0.05, αvsαααp<0.05, αvsααααp<0.001, *vs*** p<0.001, **vs*** p<0.05/+vs++p<0.001/¡vs¡¡p<0.001/¿vs¿¿p<0.05/$vs$$p<0.05/#vs##p<0.05, #vs###p<0.001/@vs@@p<0.001/&vs&&p<0.05/€vs€€p<0.001. The rest of the comparisons were not significant. M-HOBE=median of head-of-bed elevation; IQR=interquartile range.
When comparing HOBE compliance by direct-observation with self-reported compliance using the checklist, 50–60% differences were observed. Checklist-reported compliance was 89.2% (BP), 86.0% (P1), 86.4% (P2) and 90.7% (P3) while direct-observation compliance was 13.8%, 25.5%, 22.7% and 31.4% respectively (p<0.001).
Factors associated with an increased HOBE compliance differed depending on the periods in the bivariate analysis. During BP only the shift had an influence on HOBE compliance, being higher during night shift (p<0.001). During P2, morning shift and presence of ET were associated with higher HOBE compliance (p<0.05). During P3, morning shift and bed without HOBE measuring device were associated with an increased HOBE compliance (p<0.05 and p<0.001 respectively) (Fig. 3). When considering data as a whole, bivariate analysis found that morning shift, presence of ET and bed without HOBE measuring device were associated with an increased HOBE compliance (p<0.05).
Factors associated with an increase of M-HOBE also differed according to the different study periods. Nursing shift was associated with increased M-HOBE, although it changed through study periods (night shift in BP, and morning shift in P2 and P3) (p<0.05); the presence of ET was associated with higher M-HOBE in all periods except P3 (p<0.05); the presence of bed without HOBE measuring device was associated with a higher M-HOBE in all periods except P2 (p<0.05) (Table 1). When considering data as a whole, morning shift, presence of ET and bed without HOBE measuring device were associated with higher M-HOBE (p<0.05).
The multivariate logistic regression model identified presence of tracheostomy (OR 0.69, IC95% (0.57–0.85) p<0.001), afternoon shift (OR 0.77 IC95% (0.63–0.94) p<0.01) and the presence of HOBE measuring device (OR 0.78 IC95% (0.67–0.94) p<0.01) as the factors independently associated with lower HOBE compliance (Table 2).
Variables independently associated with HOBE compliance in patients with mechanical ventilation (multivariate logistic regression model).
| Variable | Odds ratio | Confidence interval 95% |
|---|---|---|
| Presence of tracheostomy | 0.693 | 0.567–0.848 |
| Bed with HOBE measuring device | 0.785 | 0.656–0.940 |
| Evening shift | 0.768 | 0.629–0.939 |
HOBE: head-of-bed elevation.
The present study reports the evaluation of M-HOBE and HOBE compliance during the longest follow-up period in the literature. Moreover, it is the first study that compares direct-observation compliance with checklist-reported compliance. As a summary, compliance lower than 35% was found during the study period, as well as a very significant gap between checklist-reported and direct observation compliance. Moreover, the presence of beds with a HOBE measuring device was not associated to higher compliances.
Our results are in accordance with others reported in the literature that have found a range of M-HOBE of 19.2°–28°13–15 as well as low compliances (<40%).15–18 Importantly, we found an improvement of HOBE compliance and M-HOBE after an educational intervention, which was statistically significant and was maintained over time. Similar improvements have been reported in other studies with shorter follow-up times. However, in most of them results were not sustained over time.16,19,22,23
Regarding checklist-reported and direct-observation compliance, we found a 50–60% difference, which was an unexpected finding. Since HOBE compliance was introduced as a part of the checklist 3 years before the study was performed, this self-reporting tool had been routinely used in every shift by the nursing staff of the study unit. Checklists implementation has been proven to be useful for avoiding human errors and improving patients’ outcomes and safety.25,28 However, checklists used for prolonged periods of time may turn them into a routine tool, failing in its intended purpose. Investigators hypothesize that this may have happened in this study. Published findings regarding hand hygiene compliance found similar results when comparing compliance estimation methods.29 They reported that self-reported compliance and self-administered checklists importantly overestimated hand hygiene compliance, which also happened in our study. For this reason, we believe that checklists are not the optimal method for improving compliance of measures that have to be implemented continuously such as HOBE, and we would recommend complementing them with random audits and feedback of the results to the clinical staff in order to encourage compliance optimization.
When analysing HOBE compliance and M-HOBE, we found that the presence of ET was associated with an increase in M-HOBE and HOBE compliance, which is in accordance with other studies.18 Variations in sickness severity along ICU stay may explain this finding. Tracheostomy is normally performed after a prolonged period of MV, once vital signs are stable. Stabilization may lead to prioritization of nursing attention to other areas of patient care other than backrest position measurement, such as patient's comfort or weaning.
We also found an influence of nursing shifts in M-HOBE and HOBE compliance, although it differed from period to period. During BP and P1, the night shift exhibited the highest M-HOBE, while morning shift was the highest during P2 and P3. We attribute this finding to a new protocol that has been implemented in our unit for improving patient's safety that includes HOBE compliance evaluation. The protocol is only performed during the morning shift and started after P1; hence we believe that this might have influenced the increase in HOBE compliance and M-HOBE during morning shifts observed in P2 and P3.
Surprisingly, and contrary to the existing evidence,23,30 we found that patients in beds without a HOBE measuring device had higher backrest elevation than the ones lying on beds with HOBE measuring device. Moreover, absence of HOBE measuring device was independently associated with HOBE compliance in the multivariate logistic regression analysis. When confronted with these results, staff nurses pointed out that visual perception of the beds with the device was somehow higher compared to the ones without it. Multiple explanations might have contributed to this observation bias, such as the pillow, the mattress type, obesity or abdominal perimeter; however, most of them are beyond the investigators control.
We expected to find lower HOBE compliance during weekends compared to weekdays. Frequently, higher percentages of unexperienced nurses work during weekends, and Vinagre et al.18 reported that experience has an impact on HOBE compliance. However, we did not find significant differences in HOBE compliance between weekdays and weekends, but it is unknown whether differences in experience were present across these two periods, as experience was not recorded during the present study.
We acknowledge that our study has several limitations. We included observations rather than patients; therefore we could not assess the impact of HOBE in VAP prevention. The compliance of the HOBE could be overestimated due to the punctual observation of the HOBE as has been demonstrated by Wolken et al. rather than continuous evaluation.22 Moreover, the number of variables studied was limited, and 18.9% of the measures could not be recorded unfortunately due to the lack/unavailability of study investigators during certain periods. Variables related to the nurse responsible for the patient, such as reasons for not following HOBE recommendations, could not be obtained due to the blinded fashion of the study. The blinded fashion also limited very importantly the number of variables that could be evaluated, as data collection was quick for not raising nurse's awareness. Moreover, this study is a single centre study, what limits the representativeness of the results. However, among our strengths we include the blinded observation to clinical staff, the comparison between checklist-reported compliance and direct-observation compliance and the one-year period follow-up.
According to our results, HOBE compliance is below optimal values and the use of checklist does not reflect the reality. Regarding risk factors for non-compliance, extra efforts are required in the nursing management of tracheostomized patients and in the correct HOBE visual perception by the nurse. The nursing shift should be also considered as an influencing factor and further analyzed to avoid differences in HOBE compliance.
In conclusion, we found an increase in M-HOBE and HOBE compliance after a formative session that remained for a year of follow-up. Checklist-reported compliance is not a good indicator for the evaluation of the HOBE compliance and is associated with important overestimation. Patients with ET had higher backrest elevation and HOBE compliance. The presence of beds with a HOBE measuring device was associated with neither an increased compliance nor M-HOBE. Nursing shift also had an influence in the HOBE compliance and M-HOBE but it changed over the time.
AuthorshipAll the authors have contributed actively in the data collection and have critically reviewed and approved the manuscript, Maria Jiménez and Alejandro Rodriguez have contributed to the data analysis, and Mireia Llaurado has participated in all the procedures, analysis and manuscript writing.
Financial support and previous diffusion of the resultsPresented partially in the “Annual National Congress of the Spanish Society of Intensive and Critical Care Nursing”, 2013 and “Annual Congress of the European Society of Intensive Care Medicine”, 2013.
Partially funded by the Research grant “Premio H.U. Marqués de Valdecilla, de investigación en enfermería”.
Conflicts of interestAll the authors declare to have no conflicts of interest with the present manuscript.
We want to thank all the nurses from the ICU for their collaboration in the study, and especially Dr Alberto Sandiumenge, Dr Christer Axelsson and Ms Elsa Afonso for their help in the critical review of the manuscript and English improvement.
Mireia Llauradó-Serra; Rosa Güell-Baró; Barbara Coloma-Gómez; Luz María Vallejo-Henao; Soledad Molina-Ramos; Laura Bordonado-Pérez; Maria Luisa Fortes-Del Valle; Margarita Peralvo-Bernat; Judith Mariné-Vidal; Yolanda Alabart-Segura; Sonia Hidalgo-Margalef; Carmen Portal-Porcel; Xavier Alabart-Lorenzo; Ascensión López-Gil.