Targeted temperature management (TTM) through induced hypothermia (between 32−36°C) is currently regarded as a first-line treatment during the management of post-cardiac arrest patients admitted to the Intensive Care Unit (ICU). The aim of TTM is to afford neuroprotection and reduce secondary neurological damage caused by anoxia. Despite the large body of evidence on its benefits, the TTM is still little used in Spain. There are controversial issues referred to its implementation, such as the optimal target body temperature, timing, duration and the rewarming process. The present study reviews the best available scientific evidence and the current recommendations contained in the international guidelines. In addition, the study focuses on the practical implementation of TTM in post-cardiac arrest patients in general and cardiological ICUs, with a discussion of the implementation strategies, protocols, management of complications and assessment of the neurological prognosis.
Actualmente, el control estricto de temperatura mediante hipotermia inducida (entre 32°C y 36°C) se considera un tratamiento de primera línea en el manejo de pacientes con parada cardiaca recuperada que ingresan en Unidades de Cuidados Intensivos. Su objetivo es disminuir el daño neurológico secundario a anoxia cerebral. Aunque existen múltiples evidencias sobre sus beneficios, el empleo de esta técnica en nuestro país es pobre y todavía existen temas controvertidos como la temperatura óptima, velocidad de instauración, duración y proceso de calentamiento. El objetivo de este trabajo es desarrollar la evidencia científica actual y las recomendaciones de las principales guías internacionales. El enfoque de este documento se centra también en aplicación práctica del control estricto de la temperatura en la parada cardiaca recuperada en nuestras Unidades de Cuidados Intensivos Generales o Cardiológicas, principalmente en los métodos de aplicación, protocolos, manejo de las complicaciones y elaboración del pronóstico neurológico.
At present, the mortality rate of out-hospital cardiac arrest (CA) remains very high, and of the patients who survive – only 13%, according to the Spanish Out-of-Hospital Cardiac Arrest Registry (OSHCAR)1 – one-quarter do so with some type of neurological sequelae.
Few measures have been found to improve the outcomes in these patients. One of the most effective is early recognition of the clinical condition, followed by the opportune start of effective cardiopulmonary resuscitation (CPR).2 Another measure that has demonstrated a strong impact upon the patient prognosis is strict temperature control (Targeted Temperature Management [TTM]) through induced hypothermia maintained for a certain period of time. The benefits of TTM in patients recovered from defibrillable rhythm out-hospital cardiac arrest have been firmly established, and for years this technique has been regarded as first line treatment for reducing neurological damage secondary to sustained anoxia. There is also less solid scientific evidence of possible benefits of TTM in patients recovered from non-defibrillable rhythm out-hospital cardiac arrest.3
To date there had been no document in Spain compiling the evidence and adapting the existing clinical guides to the needs of the hospitals in this country. In view of this, the Spanish Society of Cardiology (Sociedad Española de Cardiología [SEC]) and the Spanish Society of Intensive and Critical Care Medicine and Coronary Units (Sociedad Española de Medicina Intensiva, Crítica y Unidades Coronarias [SEMICYUC]) recognized the need to develop a report addressing the scientific evidence, the recommendations of the main international societies, and the practical application of TTM in patients recovered from cardiac arrest in our Intensive Care Units (ICUs). This document will serve as a guide for those clinical units seeking to adopt such therapy or improve its application.
MethodologyIn order to develop the expert report, a working group of professionals at national level was established, with extensive experience in and dedication to post-resuscitation patient management based on hypothermia and temperature control. The group reviewed the available evidence and established those aspects in which consensus was complete within the group, including them as basic recommendations for those units incorporating TTM.
A PubMed search was made of all registered observational studies and clinical trials (excluding pediatric patients), using the following search terms: targeted temperature management, hypothermia, therapeutic hypothermia, cardiac arrest and neuroprotection, outcome, clinical trial, prospective study, observational study, meta-analysis. The search was limited to publications in Spanish or English, with no time restrictions. The full-text versions of all the selected articles were retrieved.
The group held a face-to-face meeting in March 2018 to review the state of the art of post-resuscitation patient management based on hypothermia and temperature control, with debate of all the identified studies and meta-analyses. In that meeting the group approved the structure of the report, with distribution of the different sections among the members for the preparation of a first draft. A second face-to-face meeting was held on 26 September to discuss this draft. The final report has been developed from the literature published up until May 2019, and has been reviewed and approved by all the signing members on occasion of the last meeting held on 23 May 2019.
The report is supported and endorsed by the SEMICYUC and the SEC.
Post-cardiac arrest neuroprotectionOne out of every 10 patients with cardiac arrest survives, though only half of those who survive do so in acceptable neurological condition. Patients surviving CA experience post-resuscitation syndrome characterized by brain damage, myocardial dysfunction, systemic ischemia-reperfusion syndrome and the clinical conditioning factors responsible for cardiac arrest in the first place.4
A number of procedures can help reduce damage secondary to general ischemia and treat post-resuscitation syndrome (Table 1).5–7
Procedures for reducing secondary neurological damage.5–7.
| Coronary angiography in patients with STEMI or with suspected cardiac arrest |
|---|
| Identification of the causal factor |
| Respiratory care, avoiding hypoxemia and hyperoxia |
| Hemodynamic monitoring with invasive arterial control, central venous access, and monitoring of cardiac output |
| Early echocardiography |
| Measurement of mixed venous saturation, lactic acid and diuresis |
| Strict monitoring of natremia, glycemia and patient head position |
| Detection and treatment of seizures |
STEMI: ST-segment elevation myocardial infarction.
Neuromonitoring based on minimally invasive techniques (brain oximetry, transcranial Doppler, imaging tests) can contribute to decision making and the early detection of cerebral hypertension or ischemia.
Neuroprotection strategies can limit secondary nervous tissue loss and improve the functional outcomes.8 There are two fundamental neuroprotection strategies: maintenance of an adequate oxygen supply and the modulation of consumption to adapt it to the offer. A number of therapeutic options are available for this purpose, including particularly TTM.9 Pharmacological neuroprotection in neurocritical patients – whether post-cardiac arrest cases or otherwise – has not yielded the desired effects.10
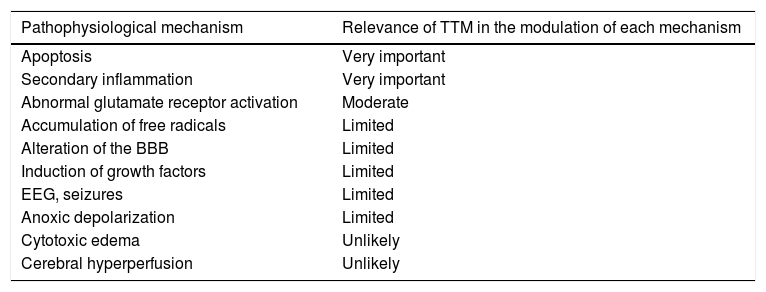
Hypothermia and neuroprotectionThe relationship between neurological damage and thermoregulation is complex. Hypothermia during hypoxia-ischemia/reperfusion acts via different mechanisms, but is fundamentally characterized by the reduction of anoxic depolarization, excitotoxicity, free radical exposure and blood-brain barrier (BBB) dysfunction.11,12Table 2 describes the different pathophysiological mechanisms in post-resuscitation syndrome following CA and the degree of influence of hypothermia in each of them.
Mechanism of action of hypothermia and relevance of TTM in each pathophysiological mechanism in post-resuscitation syndrome.11.
| Pathophysiological mechanism | Relevance of TTM in the modulation of each mechanism |
|---|---|
| Apoptosis | Very important |
| Secondary inflammation | Very important |
| Abnormal glutamate receptor activation | Moderate |
| Accumulation of free radicals | Limited |
| Alteration of the BBB | Limited |
| Induction of growth factors | Limited |
| EEG, seizures | Limited |
| Anoxic depolarization | Limited |
| Cytotoxic edema | Unlikely |
| Cerebral hyperperfusion | Unlikely |
BBB: blood-brain barrier.
Hypothermia offers different potentially beneficial effects in post-CA management: it lowers metabolic activity, thereby allowing organs to tolerate longer periods of ischemia without suffering irreversible damage, and it is able to reduce the deleterious effects of reperfusion – particularly neurological damage induced by the release of inflammatory mediators after the recovery of blood flow. In turn, hypothermia also reduces the inflammatory response and the rise in intracranial pressure, as well as the risk of fever secondary to the systemic inflammatory response (Table 2).12
TTM in post-resuscitation careThe use of TTM is recommended in all the clinical practice guides on post-resuscitation care. Although the level of acceptance and implementation of the technique is variable (in Spain it is presently used in less than 20% of all candidates1), the groups that have adopted the strategy have obtained good results.13
Aspects to be considered in TTMTarget temperature level- -
The optimum temperature level in TTM has not been defined.
- -
There is greater evidence of a favorable effect with 33°C (32−34°C) than with the standard treatment without temperature control - though there are no significant differences among three core temperature targets, namely 32–33 and 34°C.12,14–16 There is general agreement that when a target temperature of 36°C is chosen, the latter is less strictly maintained.17
- -
The study published by Nielsen et al. was designed to define a target temperature for TTM, and evidenced no differences between a temperature of 33°C versus 36°C.18 Posteriorly, the evidence showed the outcome to be poorer in patients receiving standard care in whom the target temperature was raised to 36°C.19,20 However, the appearance of fever in these patients (which worsens the prognosis) and the lax application of the hypothermia protocols are elements that do not allow us to firmly conclude that hypothermia target temperature is the factor that improves survival in the intervention group.
- -
For these reasons, an international multicenter study (Targeted hypothermia versus targeted normothermia after out-of-hospital cardiac arrest [TTM2, ClinicalTrials.gov: NCT03114033]) has been designed to compare a TTM of 33°C versus normothermia and early fever treatment (≥ 38.7°C) - with results that have not yet been published.21
- -
No trials are available on the effect of the rate of temperature reduction upon the patient prognosis. However, there are observational studies that have found no evidence indicating that the rate at which the target temperature is reached has any impact upon the clinical outcomes,22 even in those patients in which TTM is started in the pre-hospital setting.23
- -
Post-resuscitation (ischemia-reperfusion) syndrome is characterized by brain edema that causes an increase in intracranial pressure, producing additional cerebral ischemia that worsens the neurological damage already caused. There is a critical time window in this syndrome, covering the period between the recovery of spontaneous circulation and triggering of the inflammatory response, in which a decrease in body temperature may have beneficial effects. It is believed that this window may be about 4–5 hours.24
- -
The required duration of TTM is not clear. The only study in patients comparing the effect of TTM at 33°C during 24 versus 48h evidenced no superiority, though there was a tendency towards better outcomes with durations of over 24h.25
- -
To date no studies have been made on how the return to normothermia should be made, and whether it should be spontaneous or controlled.
- -
In general, when TTM is performed with the classical methods such as ice or insulating blankets, passive warming is used, since it is very difficult for warming to be made at an established rate.
- -
When feedback-based control methods are used, a controlled warming rate is commonly employed, usually between 0.1 and 0.5°C per hour, in order to avoid rebounds. Controlled normothermia should be maintained beyond the period of hypothermia, since hyperthermia phenomena are common.
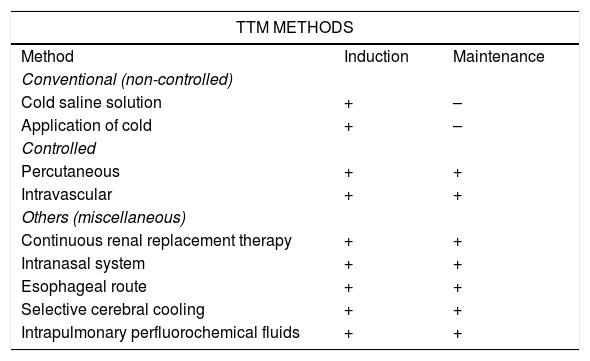
There are different methods for inducing, maintaining and reverting TTM in clinical practice. Non-controlled conventional methods, intravascular and percutaneous controlled methods, and other methods are available (Table 3).
Methods for the induction and maintenance of TTM.30.
| TTM METHODS | ||
|---|---|---|
| Method | Induction | Maintenance |
| Conventional (non-controlled) | ||
| Cold saline solution | + | – |
| Application of cold | + | – |
| Controlled | ||
| Percutaneous | + | + |
| Intravascular | + | + |
| Others (miscellaneous) | ||
| Continuous renal replacement therapy | + | + |
| Intranasal system | + | + |
| Esophageal route | + | + |
| Selective cerebral cooling | + | + |
| Intrapulmonary perfluorochemical fluids | + | + |
Comparison of these different approaches26–29 shows them to be equivalent for inducing therapeutic hypothermia, though controlled devices are more effective for maintaining TTM.30
Non-controlled conventional methodsThese methods are commonly used to induce TTM and as adjuvants to more advanced techniques.
Infusion of cold saline solution27,29The infusion of cold saline solution is simple, inexpensive and widely used to induce TTM, though it is not effective in maintaining it. The technique generally involves the use of a pressure bag to increase the infusion rate. One liter of cold saline solution infused in 15min can reduce the core temperature by 1°C. Intravenous volumes of up to two liters are used, generally in the form of 0.9% saline solution. This technique poses a risk of adverse effects in the form of overcooling, and moreover can cause volume overload and acute lung edema. It is therefore not advisable in patients with heart failure, altered kidney function, respiratory distress syndrome or evidence of volume overload.
Application of cold27,29Cold traditionally has been applied with ice bags and, more recently, with carbon-based gel pads that afford temperature reductions of 3.5°C/hour (EMCOOLS® cooling system). This rate is faster than when cold saline infusions are used (approximately 2°C/hour). The technique is simple and rapid to perform, even in the out-hospital setting, but can cause skin burns and irritation, and is not the best choice method in the presence of skin lesions (e.g., exfoliative dermatitis or extensive burns). The appearance of patient trembling associated to the drop in temperature tends to be more frequent with this technique.
Controlled methodsPercutaneous methods26,30These techniques are based on the principle of thermal conductivity. Cold liquid or air is circulated through cooling sheets, vests or pads in contact with the body of the patient.30 These methods usually lower body temperature at a rate of 0.5−1°C/hour, though the time taken to reach the desired temperature depends on the device used.
Arctic Sun® (Medivance, Bard, Beckton Dickinson, Louisville, CO, USA) is a noninvasive percutaneous system for TTM allowing faster temperature regulation and control. It controls temperatures in a range of 32–38.5°C. The operating principle is based on the circulation of cold water within a series of pads adhered to the skin of the patient. Its electronic module is connected to the disposable pads that transfer the thermal energy directly over the skin, affording isolation from the environmental temperature. This is a servo-control system that monitors body temperature each second and compares it against the desired protocol, adjusting the temperature of the circulating water 30 times an hour.
Intravascular methods26,28,30These are regarded as invasive methods. Two devices are available on the market: Thermoguard XP® (Zoll, Chelmsford, MA, USA) and InnerCool RTx® with the Accutrol® catheter (Phillips). The former system uses different central venous catheters that can be placed via the subclavian, internal jugular or femoral vein. The target temperature is reached by circulating 0.9% saline solution within a closed circuit through the catheter balloon. InnerCool RTx® uses a single type of catheter equipped with a temperature sensor for precise control. These advanced cooling systems allow computerized temperature control with a servo-control mechanism.31 With these systems the overcooling rates are lower and failure to reach the target temperature is less likely. However, the results are no better than those obtained with other techniques, and there is an added risk of intravascular infections, venous thrombosis and local complications associated with insertion of the catheters.
Other methods–Other methods include: extracorporeal cooling techniques, continuous renal replacement therapy, and bladder and esophageal cooling.30 There are concrete scenarios in which techniques other than those commented above may be chosen, depending on the patient needs and clinical condition. However, many of them are still in the early investigational stages, and adequate and larger-scale clinical studies are needed before their use can become generalized (Table 3). Esophageal cooling has been shown to be an effective maintenance option.32 Intranasal cooling in turn has been successfully used for the induction phase, though it has not improved the outcomes in terms of patient survival or neurological prognosis.33
There is grade of recommendation I with level of evidence B (based on randomized clinical trials; moderate evidence for the recommendation) for the application of TTM in patients with defibrillable rhythm out-hospital CA. Targeted temperature management should be made based on a hospital protocol defining the pertinent criteria and procedures.
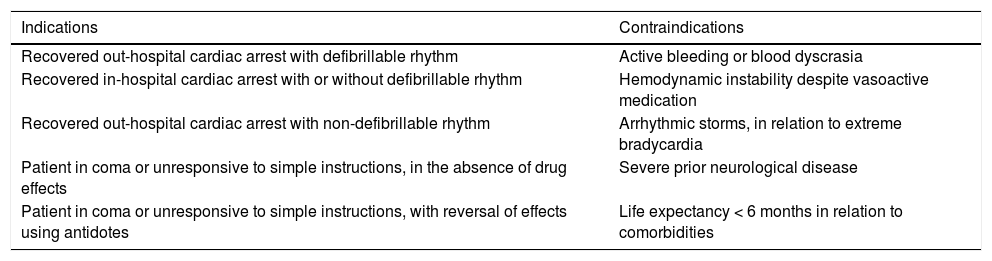
Indications and contraindicationsThe indication with the greatest scientific evidence for the application of TTM is recovered out-hospital CA with defibrillable rhythm. However, it has already been mentioned that there are other indications with a lesser level of evidence which are cited in order in Table 4. This same table also describes the contraindications of TTM, with the main complications during hypothermia – including particularly coagulopathy and the appearance of arrhythmias.
Indications and contraindications of TTM.15,34.
| Indications | Contraindications |
|---|---|
| Recovered out-hospital cardiac arrest with defibrillable rhythm | Active bleeding or blood dyscrasia |
| Recovered in-hospital cardiac arrest with or without defibrillable rhythm | Hemodynamic instability despite vasoactive medication |
| Recovered out-hospital cardiac arrest with non-defibrillable rhythm | Arrhythmic storms, in relation to extreme bradycardia |
| Patient in coma or unresponsive to simple instructions, in the absence of drug effects | Severe prior neurological disease |
| Patient in coma or unresponsive to simple instructions, with reversal of effects using antidotes | Life expectancy < 6 months in relation to comorbidities |
–Some experts advise that the delay in starting treatment should be no more than 6−12h from CA onset, though others suggest that TTM should be performed as soon as possible, without specifying any concrete time limit.
–Controlled methods are the recommended option for the entire TTM procedure. Accordingly, non-controlled methods would be useful as adjuncts only in the induction of TTM – not in maintenance.
–It is advisable to maintain TTM for at least 24h in situations of hypothermia and up to 72h from the time of the event in controlled normothermia.4,18,34
–The return to normothermia should be made in a controlled and active manner, with a warming rate of between 0.2°C/h and 0.5°C/h,34 and a target temperature of 36.5−37°C35 The latest European recommendations for the application of TTM advise a slow warming rate of 0.15−0.25°C/h.36
Patient monitoring should include6:
- a
Invasive blood pressure monitoring with an arterial catheter and the maintenance of mean blood pressure (MBP) values ensuring a cerebral perfusion pressure > 60mmHg (in most cases the value is in the order of 80mmHg, as is applied in the general management of neurocritical patients). Cerebral autoregulation status should be taken into account.
- b
Pulsioximetry. A value of 94-98% should be maintained in order to avoid hyperoxemia.6,37
- c
Bispectral index (BIS): monitoring of patient waking state – this being particularly useful in patients subjected to muscle relaxation.
- d
Continuous ECG monitoring to control rhythm and ensure the early detection of any alteration.
- e
Continuous EEG monitoring, recommended especially in patients subjected to neuromuscular block, in order to detect possible myoclonus.
Hypothermia increases the risk of bleeding and the need for blood transfusions, due to alteration of the coagulation parameters that occurs from a 0.5°C drop in temperature.39
Infectious complicationsInfectious complications are frequent (seen in up to 70% of all cases) and are favored by post-CA inflammatory syndrome and the attenuated immune response secondary to hypothermia. The absence of fever impedes the early diagnosis of infection; the incidence of sepsis is therefore almost two-fold higher in the presence of hypothermia (13% versus 7%).14 Pneumonias are the most common processes (85%). They are generally not associated to increased mortality.39
Water-electrolyte and metabolic disordersSympathetic tone rises during hypothermia, resulting in vasoconstriction and the reduction of organ perfusion. This in turn favors the development of metabolic acidosis, with a decrease in pH (from 7.37 to 7.31) and an increase in lactate concentration. The decrease in metabolic demand3,39 can imply an increase in CO2 and ventilation changes during the warming phase that could cause cerebral vasoconstriction.
Hyperglycemia is common as a result of diminished insulin output,41 though treatment is not advised in the presence of glycemia values of under 180mg/dl, in order to avoid hypoglycemia.
Hypopotassemia and hypomagnesemia are observed during cooling, and this in turn favors the appearance of potentially fatal ventricular arrhythmias. Both ions therefore require monitoring.31
Cardiovascular complicationsHypothermia has direct effects upon the heart, such as ECG alterations (prolongation of the PR interval, widened QRS and QTc) and the appearance of arrhythmias. Heart rate may also be seen to increase (at the start of TTM), followed by sinus bradycardia (40–45 bpm) that lowers cardiac output by 25-40%.39,41 However, there have been no reports of hemodynamic instability as a direct consequence of hypothermia.42
ShiveringShivering is one of the most common phenomena seen during the induction of TTM. It is a normal physiological response to lowered body temperature, seeking to produce warmth, and is associated to an increase in oxygen consumption of 50-400%. Shivering appears mainly when the temperature falls to between 35−37°C; once the target temperature of 32−34°C is reached, it becomes less frequent.43 Shivering is accompanied by hypertension, an increased heart rate and vasoconstriction, and complicates the cooling phase.39
Shivering should be prevented on an early basis. The treatment options in this regard include44: antipyretic / antiinflammatory drugs, vasodilators, opioids, alpha-agonists (dexmedetomidine), anesthetics and sedatives, serotonin agonists and neuromuscular relaxants.
The administration of magnesium sulfate at a dose of 0.5−1mg/h via the intravenous route (serum target concentration: 3−4mg/dl)45 increases the cooling rate and is convenient when percutaneous controlled methods are used – reducing smooth muscle tone and subsequent vasodilatation, with a decrease in shivering. As an added benefit, magnesium sulfate offers neuroprotective properties as an N-methyl-D-aspartate (NMDA) agonist. Although shivering control with magnesium sulfate is usually less pronounced than that afforded by sedatives or opioids, its few adverse effects make it an attractive option for use.
Opioids are the most widely used drugs (e.g., fentanil, morphine, meperidine). Meperidine is possibly the most effective option and exerts synergistic action with buscapine in suppressing shivering. However, the possible appearance of seizures or kidney damage associated to the combined use of these two drugs must be monitored.44,45 Alpha-agonists such as dexmedetomidine reduce the appearance of shivering, though their use is limited by the induction of bradycardia and hypotension.
Sedatives in combination with opioids are usually required, titrating the dose according to the suppression of shivering. The options in this regard include propofol and benzodiazepines. Neuromuscular relaxants can be used in severe cases. However, it must be taken into account that relaxants can mask the appearance of seizures, which often manifest post-CA patients.
Effects on drug pharmacokineticsIt must be taken into account that TTM induces changes in drug absorption, kinetics and metabolism; such situations must be known in order to modify therapy in these patients.42,46
Neurological prognosis after cardiac arrest and temperature managementMost patients that survive cardiac arrest are in coma immediately after the recovery of circulation, as a consequence of the transient diffuse brain ischemia. One out of every three experience delayed recovery of consciousness (72h after the start of TTM and the suspension of sedation), and 23% remain in coma one week after admission.47 On the other hand, between 15-30% of all patients with a good prognosis regain consciousness between 48h and 10–12 days after the suspension of sedation.
The early definition of a functional prognosis capable of distinguishing between slow awakening and irreversible or catastrophic damage in a structured and multimodal manner is essential in order to adjust therapeutic effort.47–49 The functional prognosis is established between 3–6 months after the episode. A poor functional prognosis includes death due to neurological causes, vegetative state and severe disability.
Tools for establishing the neurological prognosisClinical evaluation. This is the reference tool for decision making. A standardized approach is required, based on written protocols, with registry in the case history and repeated explorations.49 The physical exploration is of crucial usefulness in establishing the prognosis, particularly the motor dimension of the Glasgow coma score (GCS), with pupil and corneal reflexes.
Electroencephalography (EEG.)50 This is an advisable technique. It is not influenced by the usual temperatures of TTM, but can be affected by sedative agents. Furthermore, EEG is important for discarding non-convulsive status epilepticus – a treatable condition that worsens the patient prognosis.51
Evoked potentials. This is the most reliable tool for predicting the neurological outcome in post-CA patients subjected to TTM, with a false-positive rate (FPR) of 0.4% (confidence interval [CI]: 0-2%).49
A recent meta-analysis found clinical evaluation at the patient bedside (point of care) and the recording of evoked potentials to be useful in predicting the neurological outcome of patients subjected to TTM – the specificity performance being better when carried out after 72h.52
Near-infrared spectroscopy. No clear role has been defined for this technique in establishing the neurological prognosis following out-hospital CA.53
Biomarkers. These markers evaluate neuronal damage, are easy to determine, and the results are independent of patient sedation.47
Imaging tests. Computed axial tomography (CAT) is essential in the presence of traumatic brain injury (TBI) or bleeding damage, and in the early diagnosis of brain ischemic injury after 24h.
According to the meta-analysis published by Golan et al. in 2014,52 the three tests that predict a poor outcome with a low false-positive rate (FPR) are: absence of pupil reflexes during > 24h (FPR: 2% [CI: 1-6%] but with low sensitivity), absence of corneal reflexes during > 24h (FPR: 4% [CI: 1-9%]), and the bilateral absence of evoked potentials (FPR 3% [CI: 1-7%]). Other tests with poorer FPR performance are GCS<2 (high sensitivity of 70-80% but low specificity), EEG patterns indicative of poor prognosis, myoclonus, and elevated enolase concentrations at 72h. It is also important to consider the factors associated to a good prognosis, such as EEG with early reactivity in the first 12h, auditory reactivity in the EEG study on the second day, and a magnetic resonance imaging (MRI) scan without diffusion alterations in the first week.
According to the guides of the European Resuscitation Council and the European Society of Intensive Care Medicine (ERC-ESCIM) 2014,48 evoked potentials with the absence of N20 components offer good discriminating capacity under conditions of normothermia. Electroencephalography is of great value with a lack of reactivity and the presence of burst suppression, but should not be used before 72h, due to the risk of interference from TTM and sedation. Furthermore, EEG should be used together with other tests. The data referred to the validity of neuroimaging, biomarkers or both are inconclusive or limited.52,54
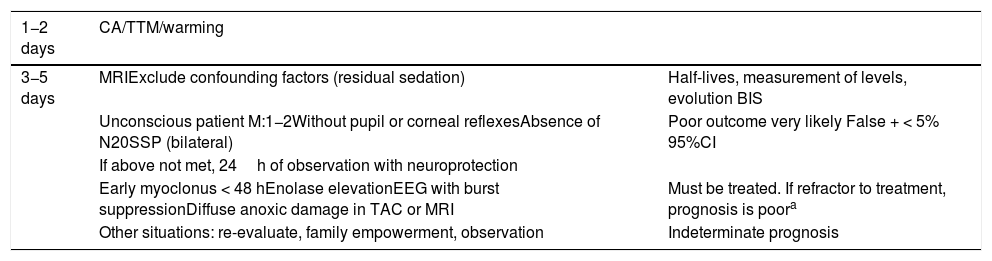
Multimodal approachThe most widespread recommendation for establishing a neurological prognosis is the adoption of a multimodal approach comprising different clinical, instrumental and laboratory test elements (Table 5).
Multimodal approach to neurological prognosis.
| 1−2 days | CA/TTM/warming | |
|---|---|---|
| 3−5 days | MRIExclude confounding factors (residual sedation) | Half-lives, measurement of levels, evolution BIS |
| Unconscious patient M:1−2Without pupil or corneal reflexesAbsence of N20SSP (bilateral) | Poor outcome very likely False + < 5% 95%CI | |
| If above not met, 24h of observation with neuroprotection | ||
| Early myoclonus < 48 hEnolase elevationEEG with burst suppressionDiffuse anoxic damage in TAC or MRI | Must be treated. If refractor to treatment, prognosis is poora | |
| Other situations: re-evaluate, family empowerment, observation | Indeterminate prognosis |
CA: cardiac arrest; MRI: magnetic resonance imaging; CAT: computed axial tomography; TTM: targeted temperature management.
The recommendations of the group of experts are described below.
Temperature control and neuroprotection–Temperature control has been the fundamental strategy for providing neuroprotection in patients with post-cardiac arrest syndrome in the last 15 years.
–Pharmacological neuroprotection in neurocritical patients – whether post-cardiac arrest cases or otherwise – has not yielded the desired effects.
–Based on the existing evidence, strict temperature control between 32−36°C is recommended in comatose patients recovered from cardiac arrest. The evidence is greater with lower temperature levels.
–The selected temperature level should be maintained for at least 24h. Some studies report better results with even longer treatments.
–Warming should be controlled between 0.2−0.5°C per hour, with the active maintenance of normothermia for at least 24 additional hours.
–Before choosing the ideal temperature control method, a number of factors must be taken into account, applying technical knowledge and considering the availability and applicability required by each option, and which can have a relevant influence upon treatment effectiveness.
–When TTM is applied, the appearance of shivering associated to hypothermia usually requires the use of sedation and neuromuscular block.
–Both percutaneous and intravascular methods are effective for maintaining the recommended temperature during 12−24hours, though due consideration is required of the greater precision of devices that regulate temperature on a constant basis, and of the risks associated to the use of invasive devices.
–Depending on the experience of the hospital center, it is common to use two or more temperature control methods simultaneously to reduce temperature. Nevertheless, the risks of exceeding the therapeutic limit must be considered, and undue patient risk is to be avoided.
–The conventional methods (ice, water blankets, etc.) have no autoregulatory capacity; therefore, while they may be useful for helping with the cooling rate, they are not advised for maintaining the temperature, in view of their poor precision and handling difficulties.
–Controlled methods are indicated for the induction (in combination or not with conventional methods) and maintenance of temperature control, with no significant differences in clinical outcome between them. Both strategies (percutaneous and intravascular) are valid, though due consideration is always required of the patient risks associated with invasive approaches.
–Intranasal cooling has been successfully used for the induction phase, but has not improved the outcomes in terms of patient survival or the neurological prognosis.
–Other methods include: extracorporeal cooling, continuous renal replacement therapy, and bladder and esophageal cooling.
–Esophageal cooling has been shown to be effective for maintenance.
–It is necessary to establish a protocol clearly specifying which patients will receive treatment and how it will be carried out, in order to homogenize patient management and optimize the outcomes.
–The protocol should include aspects related to the technique, the prevention of complications, general management of the patient, and neurological assessment.
–The nursing staff plays a crucial role in implementing TTM in the ICU. In this regard, the availability of professionals with good training in the technique and in patients of this kind is fundamental for success.
The company Bard BD has provided logistic support for the meetings of the experts, without influencing the content of the present report. RFR has received fees from MSD, Pfizer, Shionogi, BD, Philips, Jafron, Toray and Thermofisher. MCF has served as consultant and has been involved in information work for BD and Innovasc. The rest of the authors declare that they have no conflicts of interest.
The group of experts are grateful for the collaboration of the following specialists in conducting the review and developing the recommendations:
Amaia Martiarena-Orce. Intensivist, Complejo Hospitalario de Navarra.
Ara Murillo-Pérez. Nursing Supervisor, Intensive Care Unit, Hospital Doce de Octubre, Madrid.
Juan Carlos Ruiz-Rodriguez. Intensivist, Hospital Vall d’Hebron, Barcelona.
Erika Plata-Menchaca. Clinical researcher of the Shock, Organ Dysfunction and Resuscitation (SODIR) group of Vall d'Hebron Institut de Recerca (VHIR), Barcelona.
Ana Loza-Vázquez. Intensivist, Hospital Nuestra Señora de Valme, Seville.
Francisco Lucena-Calderón. Intensivist, Hospital Nuestra Señora de Valme, Seville.
Sandra Rosillo-Rodríguez. Staff physician, Acute Cardiac Care Unit, Department of Cardiology, Hospital de La Paz, Madrid.
Please cite this article as: Ferrer Roca R, Sánchez Salado JC, Chico Fernández M, García Acuña JM, Lesmes Serrano A, López de Sá E, et al. Manejo con control de temperatura en los cuidados posparada cardiaca: documento de expertos. Med Intensiva. 2021;45:164–174.